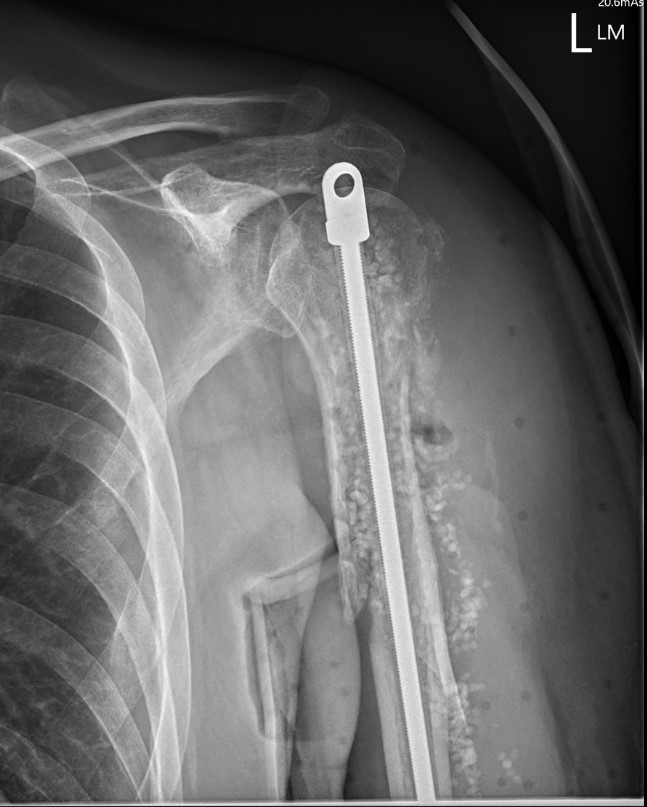
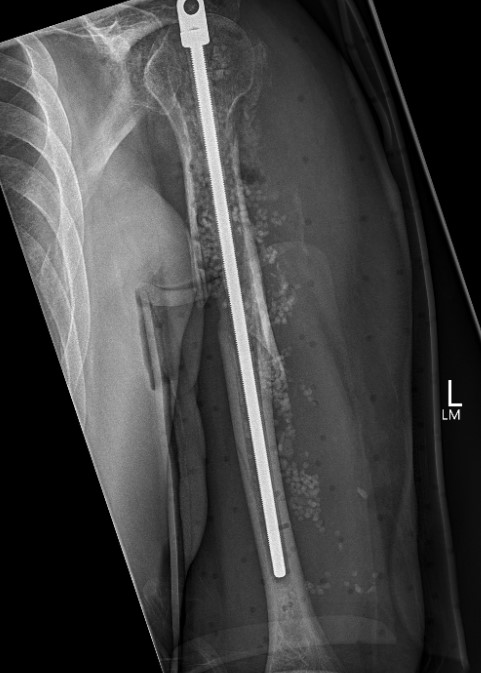
Nonoperative Management
Indications
< 20o sagittal
< 30o coronal
< 3 cm of shortening
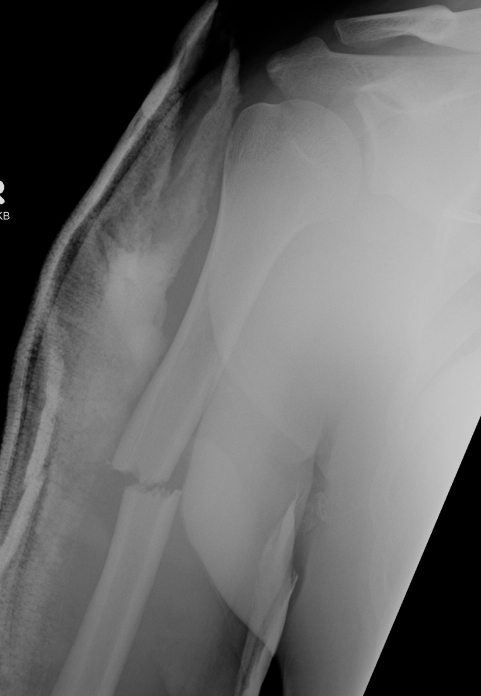
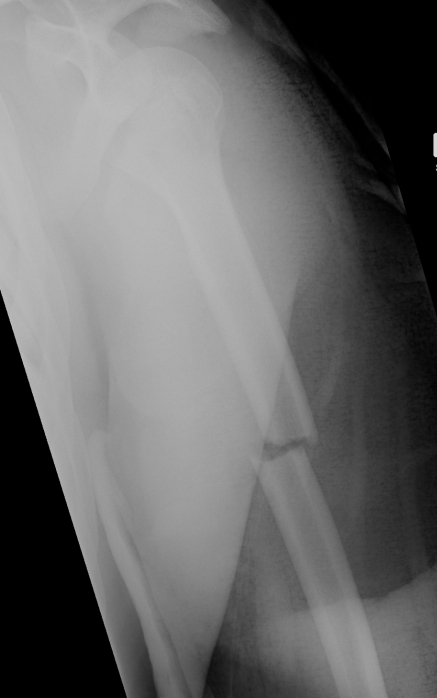
Options
1. Vietnam Cast / hanging cast
2. Functional bracing / Sarmiento
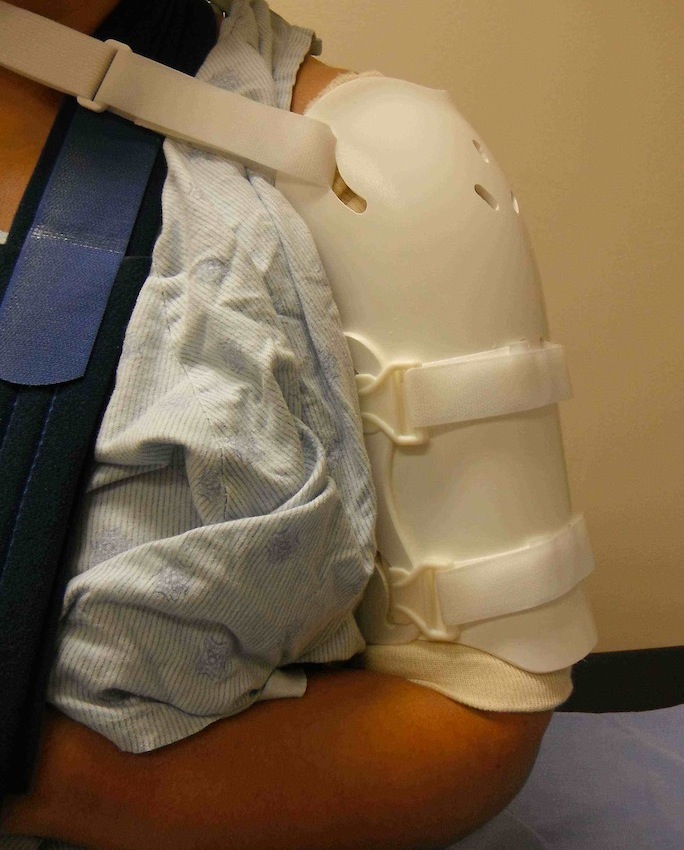
Results
Union rates
- non operative v operative treatment 213 fractures
- non operative: 20% nonunion and 12% malunion
- operative group: 8% nonunion and 1% malunion
- no difference in time to union in two groups
Ali et al. J Shoulder and Elbow Surgery 2015
- retrospective review of 138 patients treated nonoperatively
- 17% nonunion (24/138)
- proximal fractures highest nonunion rate
Time to union and functional outcome
- literature review of functional bracing humerus shaft fractures
- average time to union 10.7 weeks
- full shoulder ROM in 80%
- full elbow ROM in 85%
https://pubmed.ncbi.nlm.nih.gov/19523625/
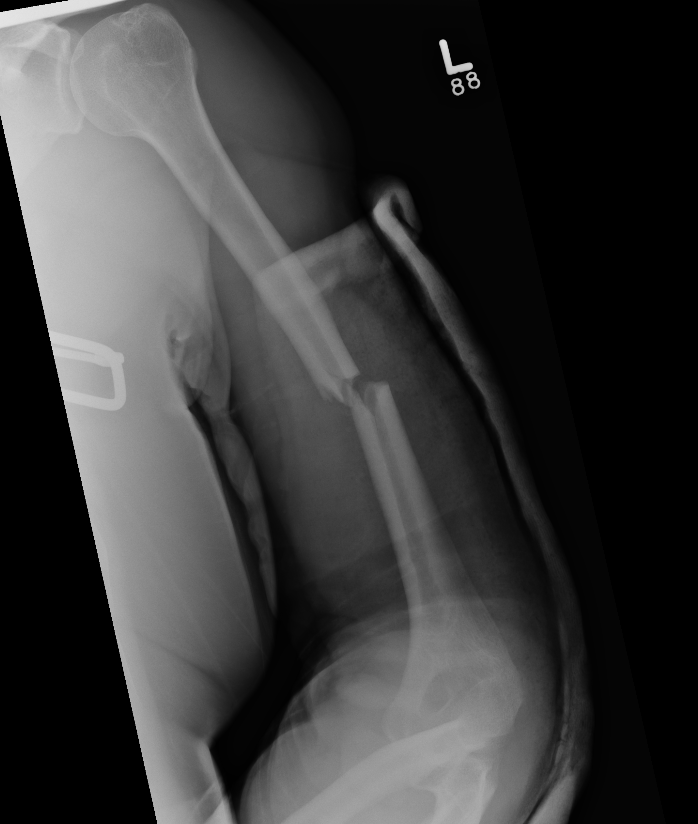
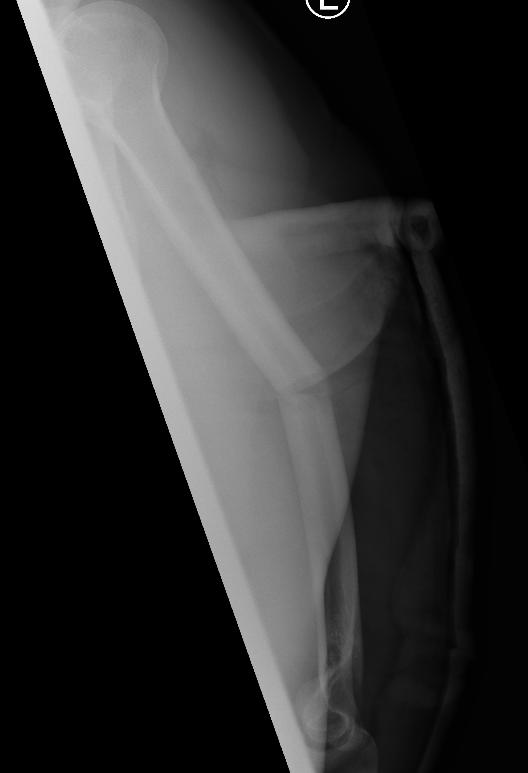
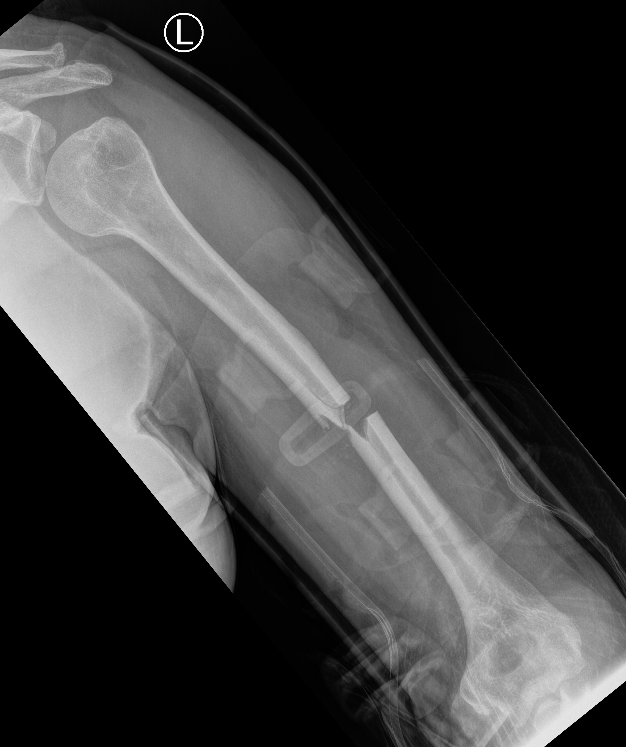
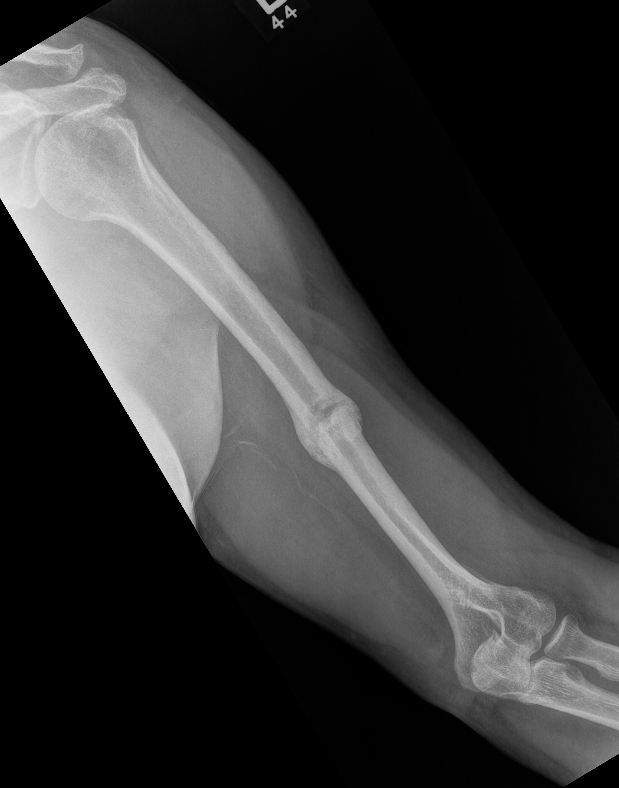
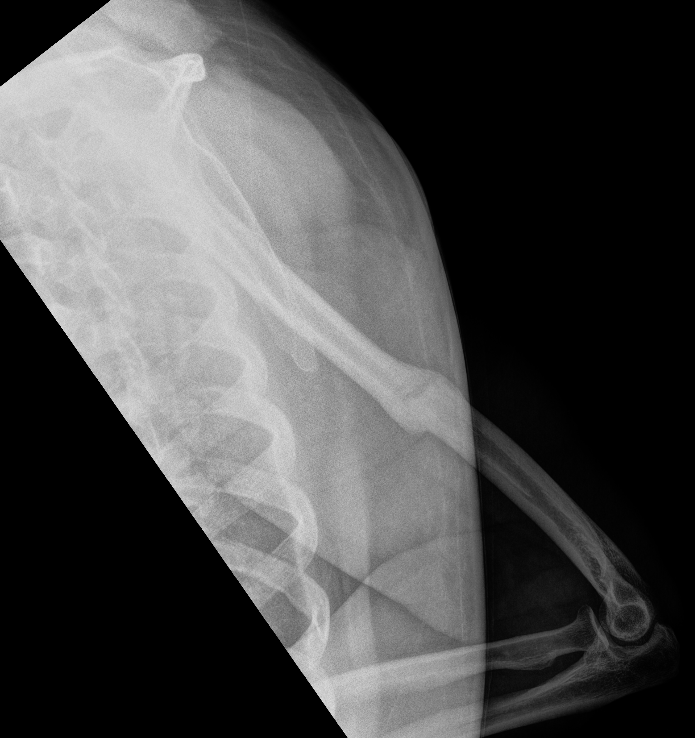
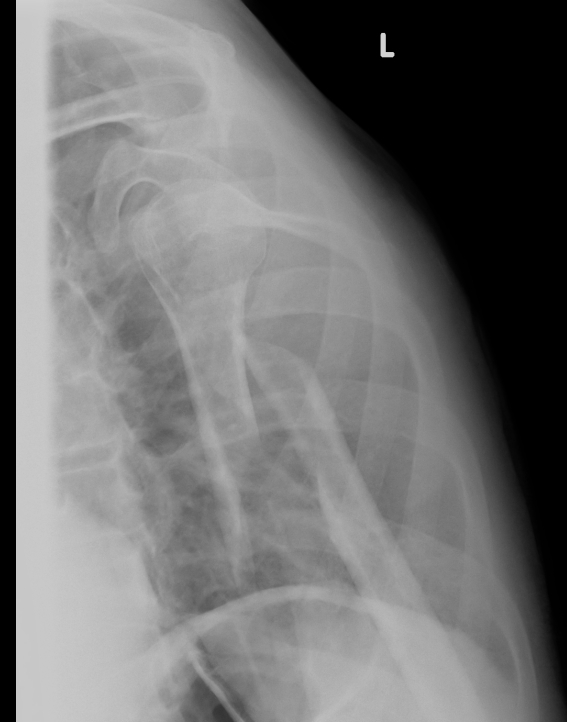
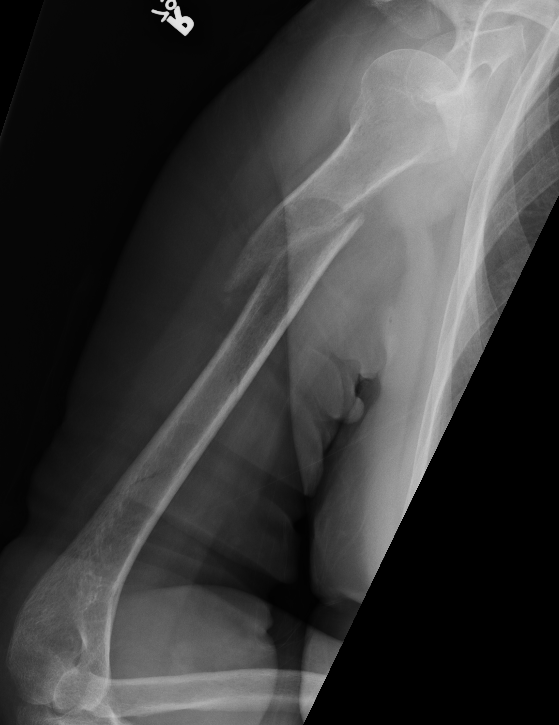
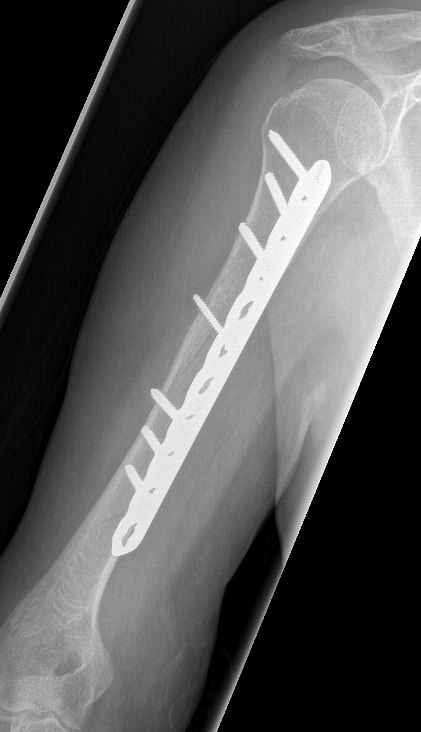
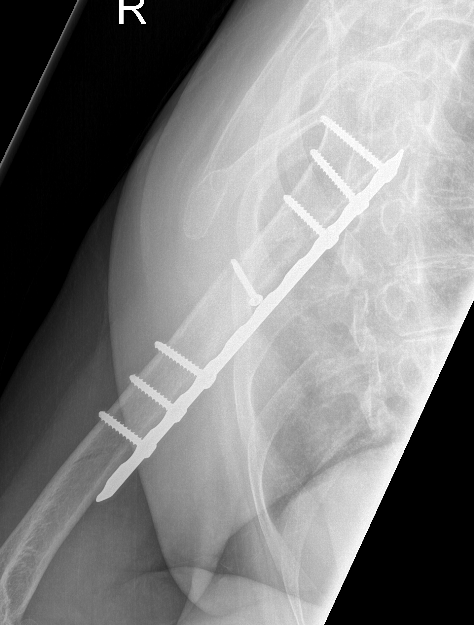
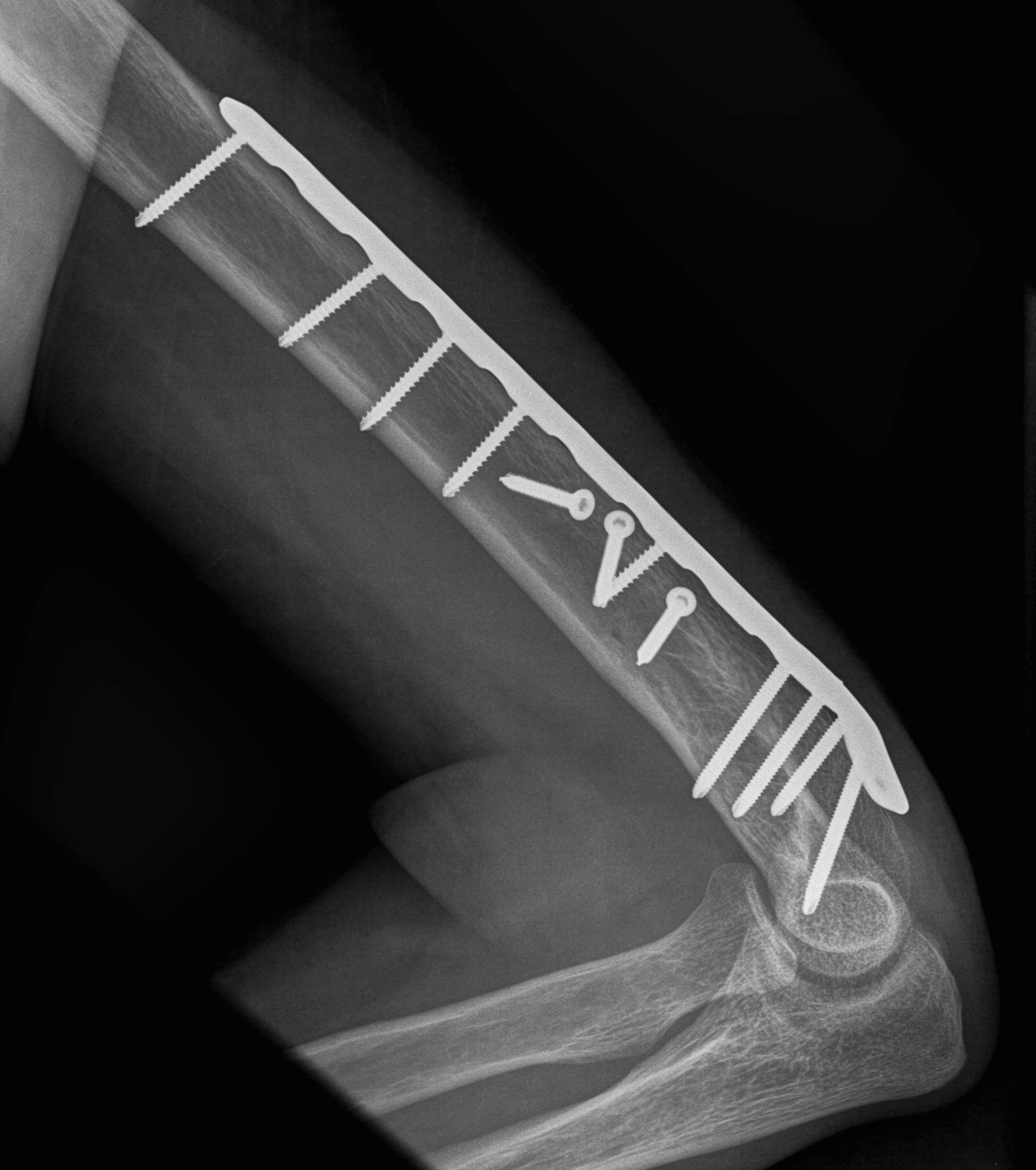
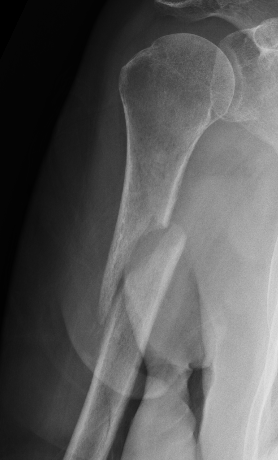
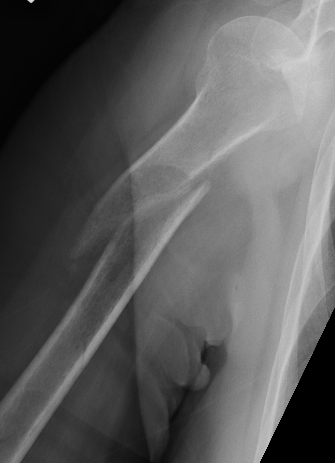
Progressive union in midshaft humerus fracture treated nonoperatively
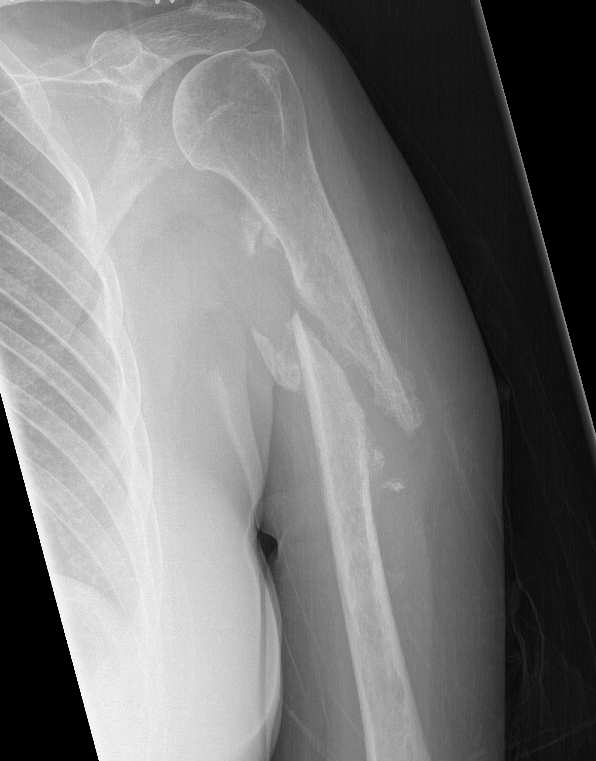
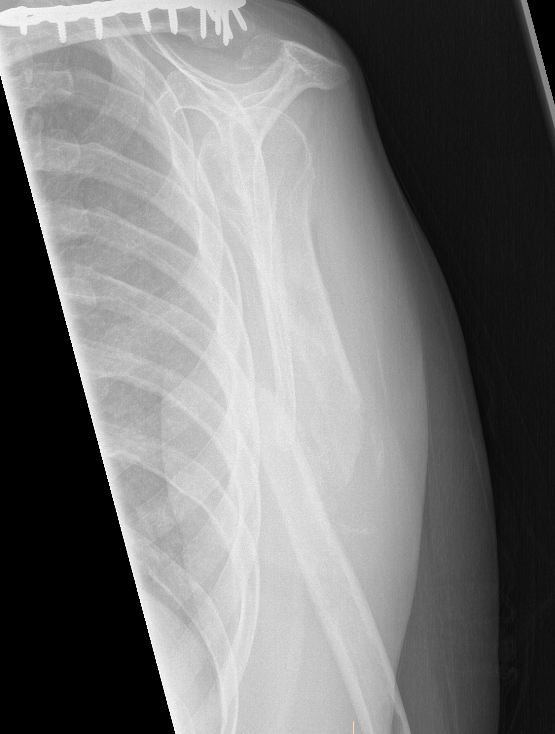
Nonunion in a proximal humerus shaft fracture treated nonoperatively
Radial Nerve Injury
Incidence
- systematic review of humerus shaft fracture
- 11.8% (532/4517) radial nerve injuries
- most common with middle, and middle/distal fractures
- 70% spontaneously recovered without intervention
- recovery rate 88% in those undergoing delayed exporation (14 weeks)
- recovery rate 88% in those undergoing immediate exploration
Holstein Lewis fracture
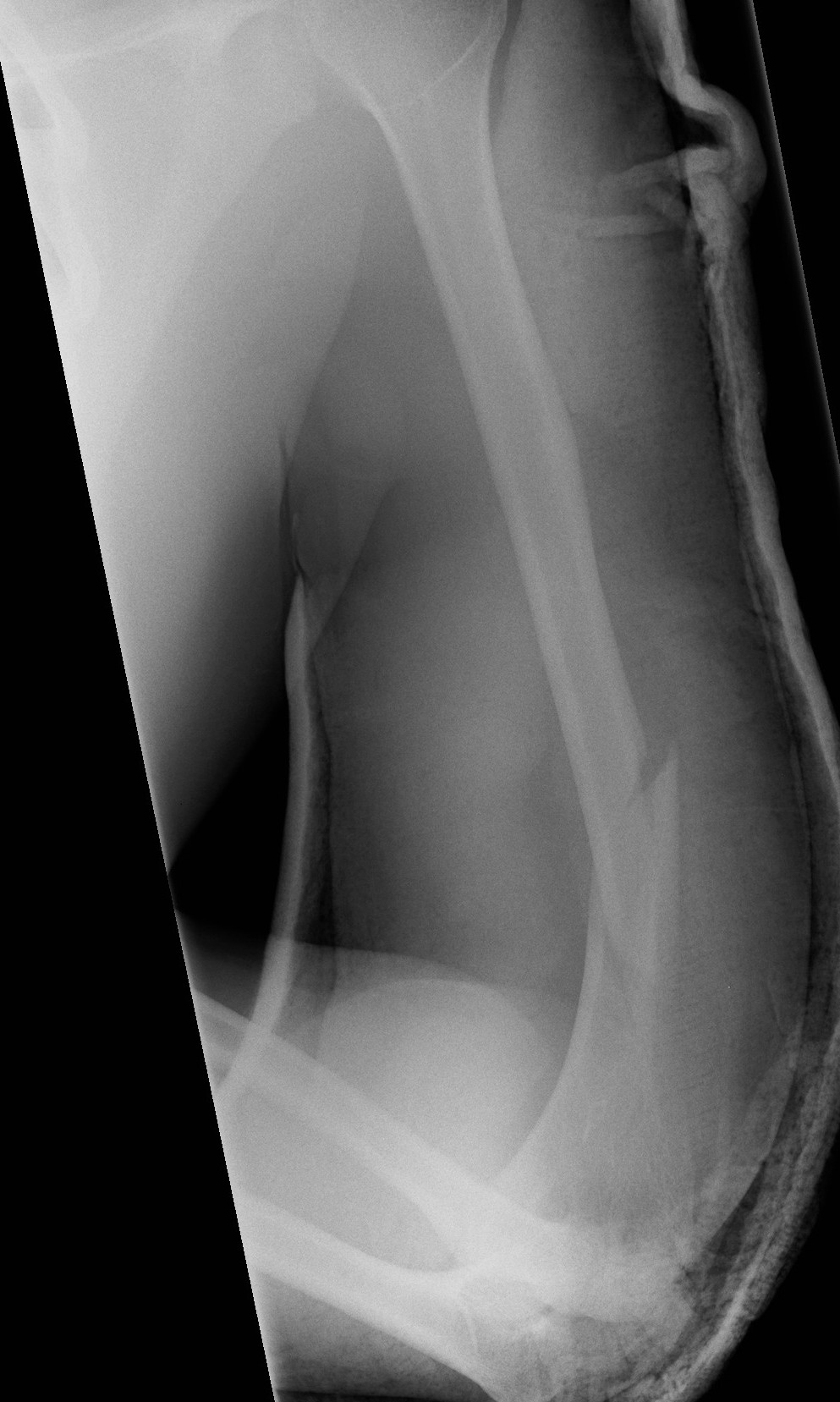
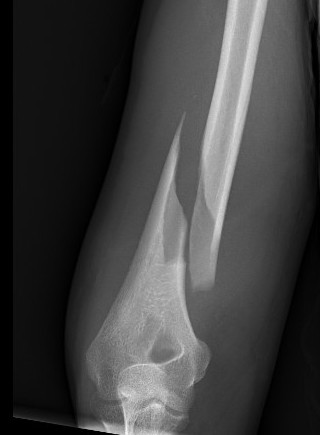
Holstein-Lewis JBJS Am 1963
- series of 7 oblique distal third fractures with radial nerve injury
- all were treated operatively
- nerve in fracture gap in 2 / impaled in 1 / severed in 2 / contused +/- in callus in 2
- advised against attempted closed reduction
- risk of contusing nerve between fragments
- advised early open reduction through anterolateral approach
- the radial nerve is closely assoicated with the fracture site and the fracture spike
Korompilias et al. Injury 2013
- 25 patients with complete nerve palsy and humerus shaft fractures
- 13 fully recovered by 12 weeks
- explored 12 patients with no recovery at 16 weeks
- nerve lacerated in two patients
- intact in remainder - these fully recovered by 20 - 24 weeks
Management
Absolute indications for exploration
- open fractures
- radial nerve palsy following closed reduction
Relative
- Holstein-Lewis fracture patterns
- patient undergoing ORIF
- no recovery at 10 - 12 weeks
Expectant management
- wait 10 - 12 weeks
- if no recovery EMG
- consider exploration +/- neurolysis +/- nerve graft at that time
- if that fails, tendon transfer for radial nerve palsy
Operative Management of Humeral Shaft Fractures
Indications
Absolute
Compound fracture
Failure to obtain / maintain acceptable reduction
Radial nerve palsy post reduction
Displaced Holstein Lewis with radial nerve palsy
Nonunion
Relative
Multi-trauma
Floating elbow
Segmental fracture
Proximal fracture
Pathological fracture - won't heal
Bilateral humeral fractures
Obese (very difficult to splint)
Brachial plexus injury - allows early rehab
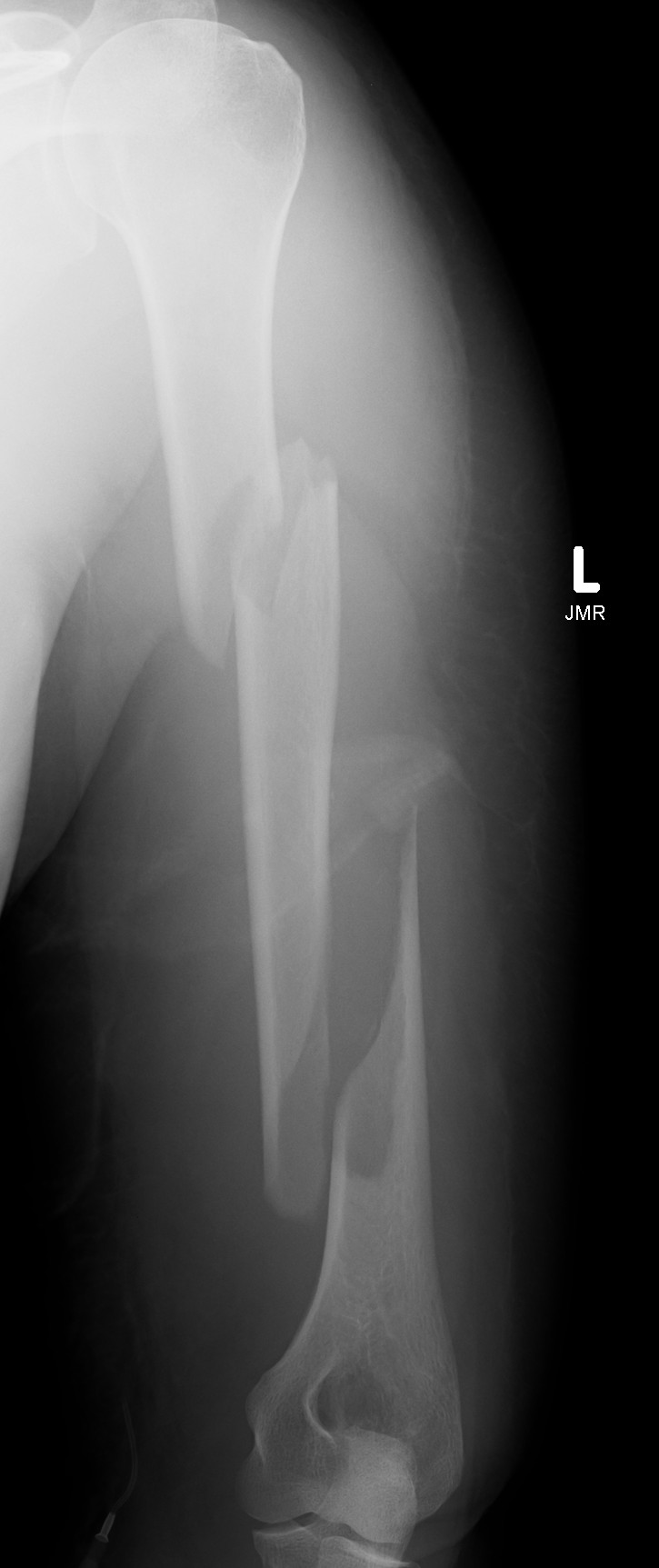
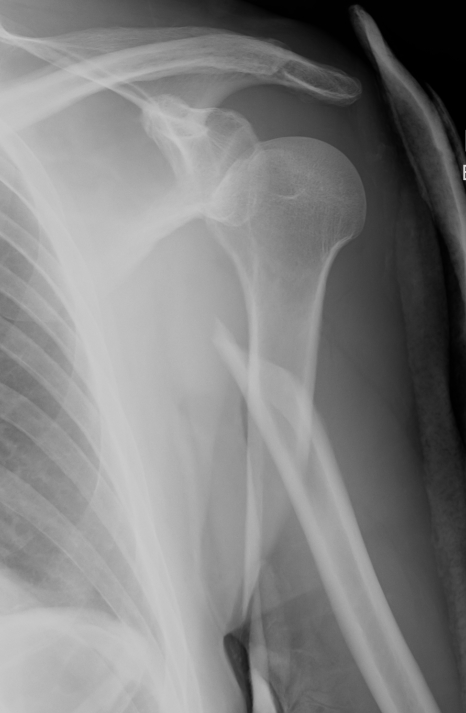
Options
Open ORIF with plate
MIPO
Intra-medullary nail
Evidence
Nail v plate
Beeres et al. Eur J Trauma Emerg Surg 2021
- IM nail v open plate
- meta-analysis of 10 RCTs (500 pts)
- SR of 18 observational studies (4900 pts)
- 17% of IMN required reoperation for shoulder impingement
- IMN had faster union and lower infection rate
- no difference nonunion rates or shoulder function scores
van der Wall et al. Eur J Trauma Emerg Surg 2021
- IM nail v MIPO
- meta-analysis of 2 RCTs (87 pts)
- systematic review of 5 observational studies (600 patients)
- MIPO lower risk of nonunion and re-intervention
- MIPO better shoulder function
ORIF v MIPO
- MIPO v ORIF
- meta-analysis of 2 RCTS (98 pts)
- systematic review of 7 observational studies (263 patients)
- MIPO lower risk of nonunion
- no difference in infection or time to union
1. Open ORIF with plate
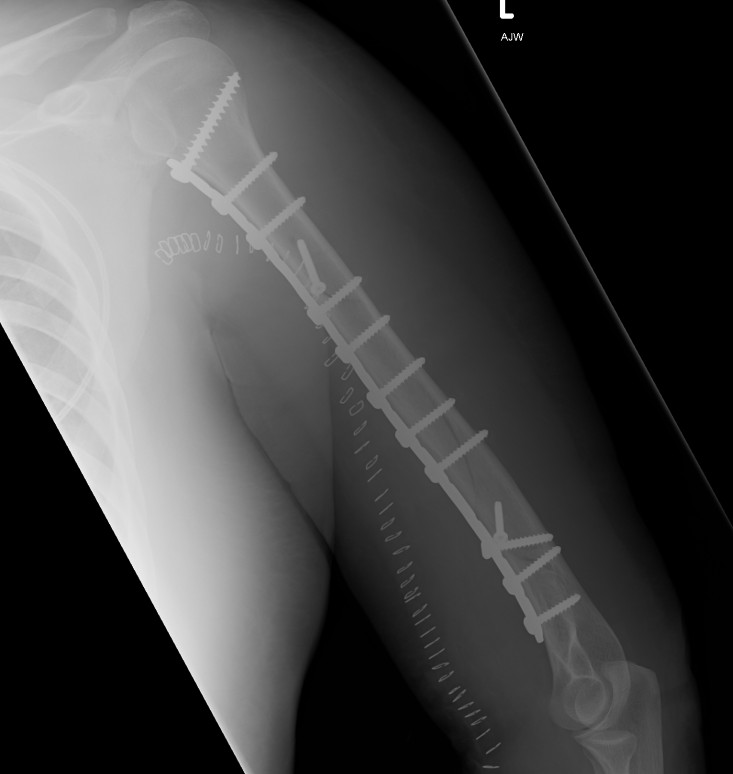
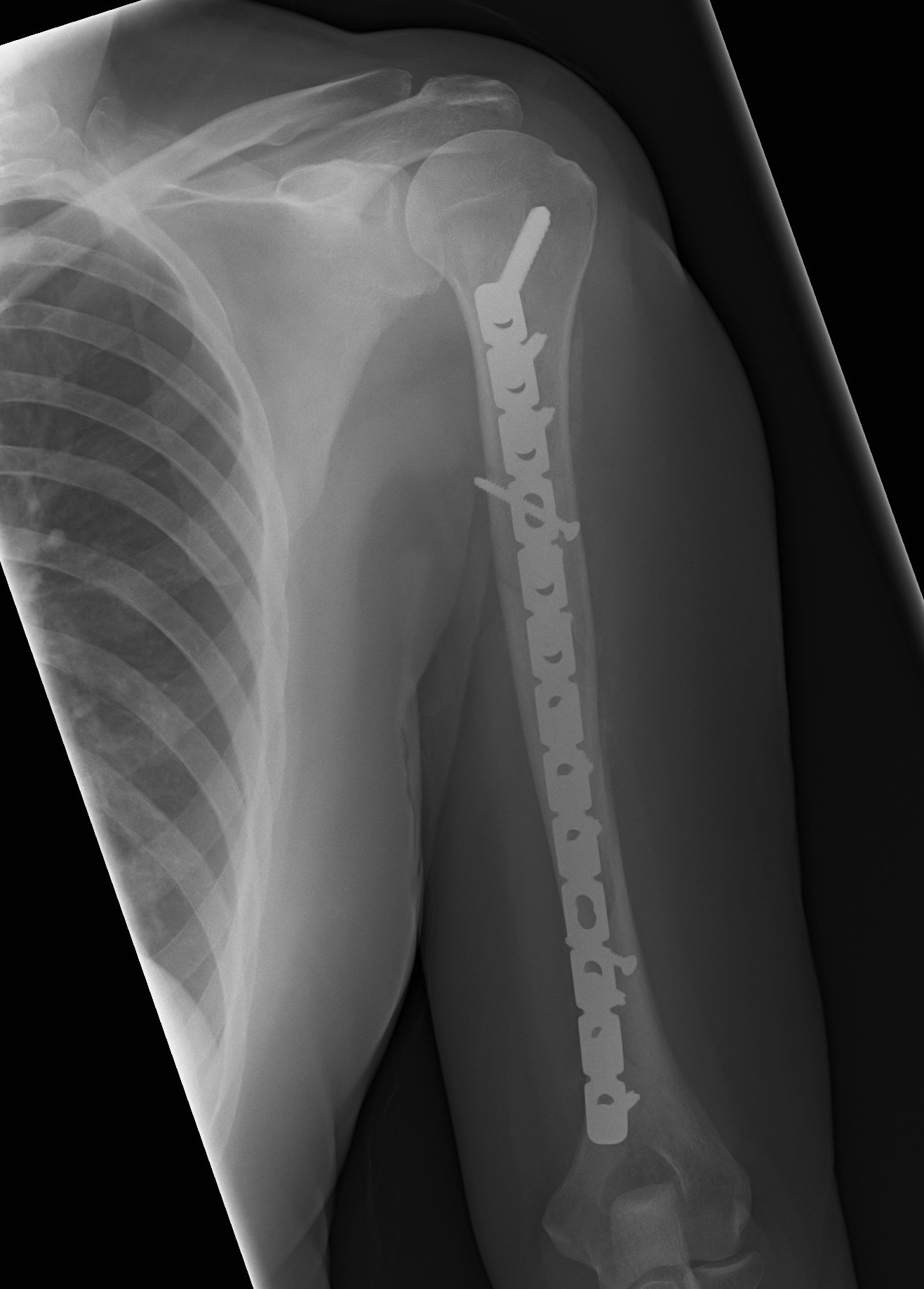
Approaches
Anterolateral approach - proximal 2/3 of humerus
Posterior approach / triceps split - distal 1/3 of humerus
Posterior approach with triceps flip - Holstein lewis
A. Anterolateral Approach Humerus for proximal / mishaft fractures
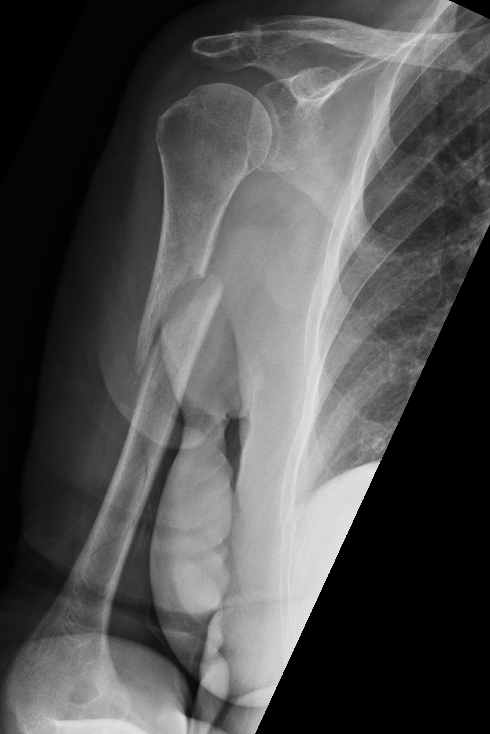
AO foundation surgical approach
Indication
- proximal fractures
- midshaft fractures
Set up
- lazy beachchair
- flat with arm on arm table
- ensure can get good images of humeral head
Incision
- deltopectoral proximally (to coracoid)
- lateral humerus distally
- distally between mobile wad and biceps
Proximally
- deltopectoral groove
- identify and protect cephalic vein
- take vein laterally to minimis bleeding
- can partially release deltoid insertion if needed
Distally
- follow cephalic
- open fascia laterally
- identify plane between biceps and brachialis
- biceps swept medially
- protect musculocutaneous nerve between the two
- will emerge as lateral cutaneous nerve of the forearm distally
- identify and split brachialis in midline
- can reflect brachialis medially, but will potentially damage radial innervation of medial brachialis
Distal extension
- between brachialis and brachioradialis in distal 1/4
- find and protect radial nerve as it emerges anteriorly through lateral intermuscular septum
- may be easiest to find radial nerve most distally between brachialis and bradioradialis
- avoid lateral hohman retractors in this area
Internervous plane
- radial nerve lateral brachialis
- musculocutaneous nerve medial brachialis
Plate
- narrow large fragment 4.5 mm DCP / long Philos proximal humeral plate
- minimum 6 cortices above and below
B. Posterior Approach and triceps split for Distal 1/3 fractures
AO foundation surgical approach
Indication
- distal 1/3 fractures
- holstein-lewis fractures
Position
- lateral approach with arm over bolster
Midline incision
- split deep fascia
Proximally
- develop interval between long and lateral heads of triceps (easiest in muscle bellies proximally)
- identify radial nerve and profunda brachii artery proximally in spiral groove
- release lateral head of triceps from humerus
- limited by axillary nerve / posterior circumflex humeral artery proximally
Distally
- split triceps tendon
- reflect medial head of triceps from bone medially
- care of ulna nerve which emerges posteriorly through medial intermuscular septum
C. Posterior approach with triceps sparing for Holstein Lewis
AO foundation radial window distal humerus
Indication
Holstein Lewis / distal humerus fracture
Approach
Patient lateral with arm over bolster
A. Mobilise the lateral triceps from lateral intermuscular septum
- identify the radial nerve lateral to triceps
- follow as it passes through the lateral intermuscular septum
- identify as passes across the humerus in the groove
- may have to elevate the radial nerve and pass the plate under
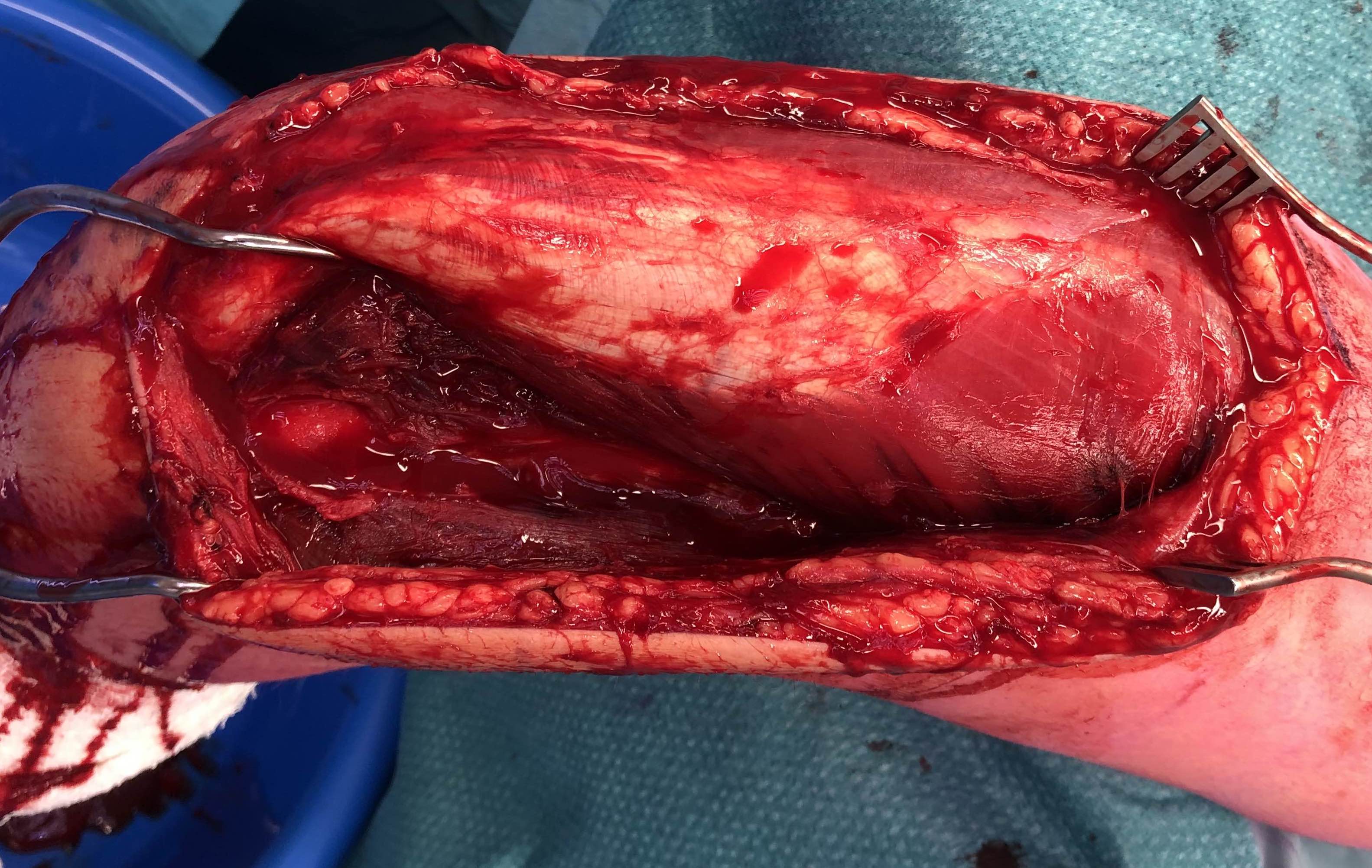
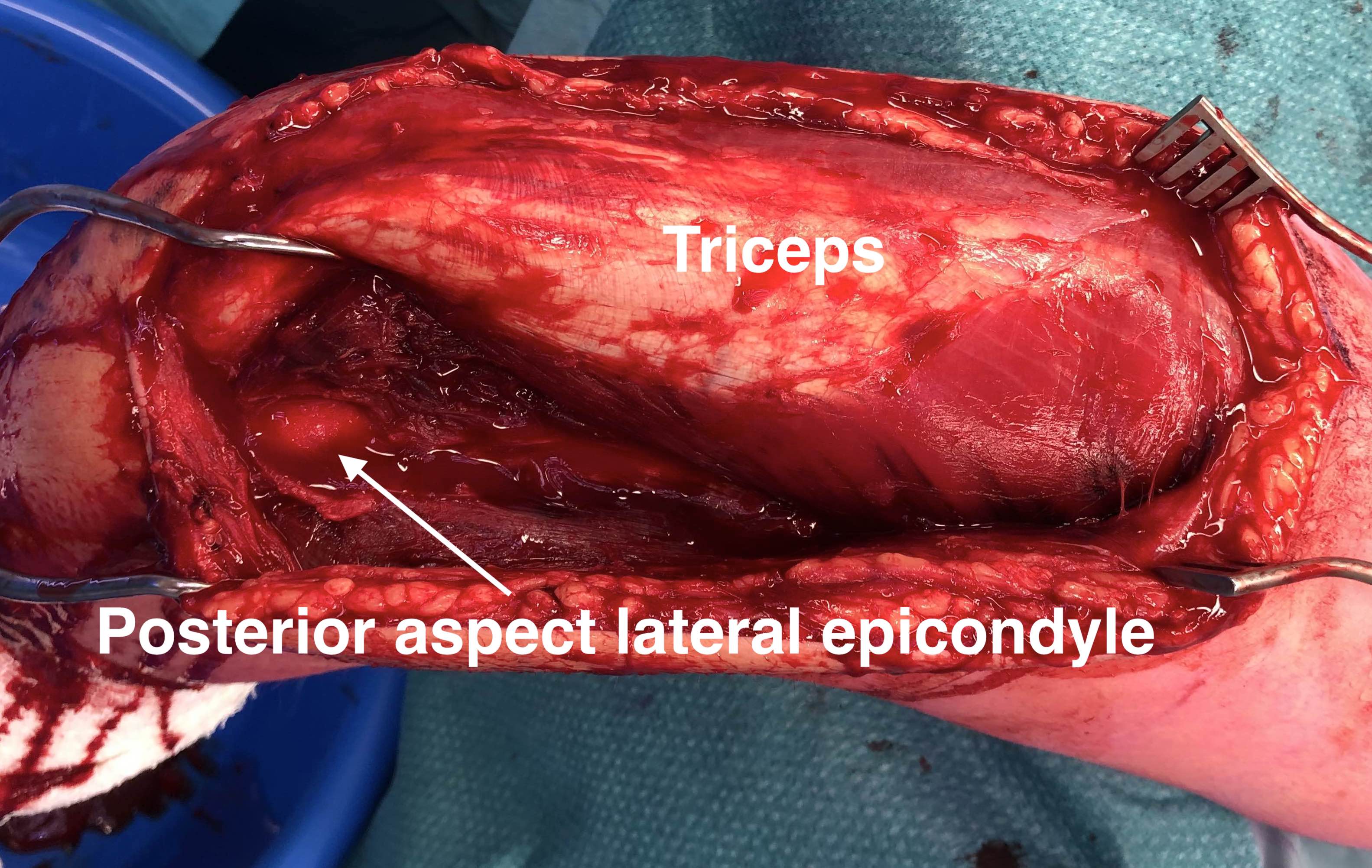
Plate
Precontoured long posterolateral distal humerus plates
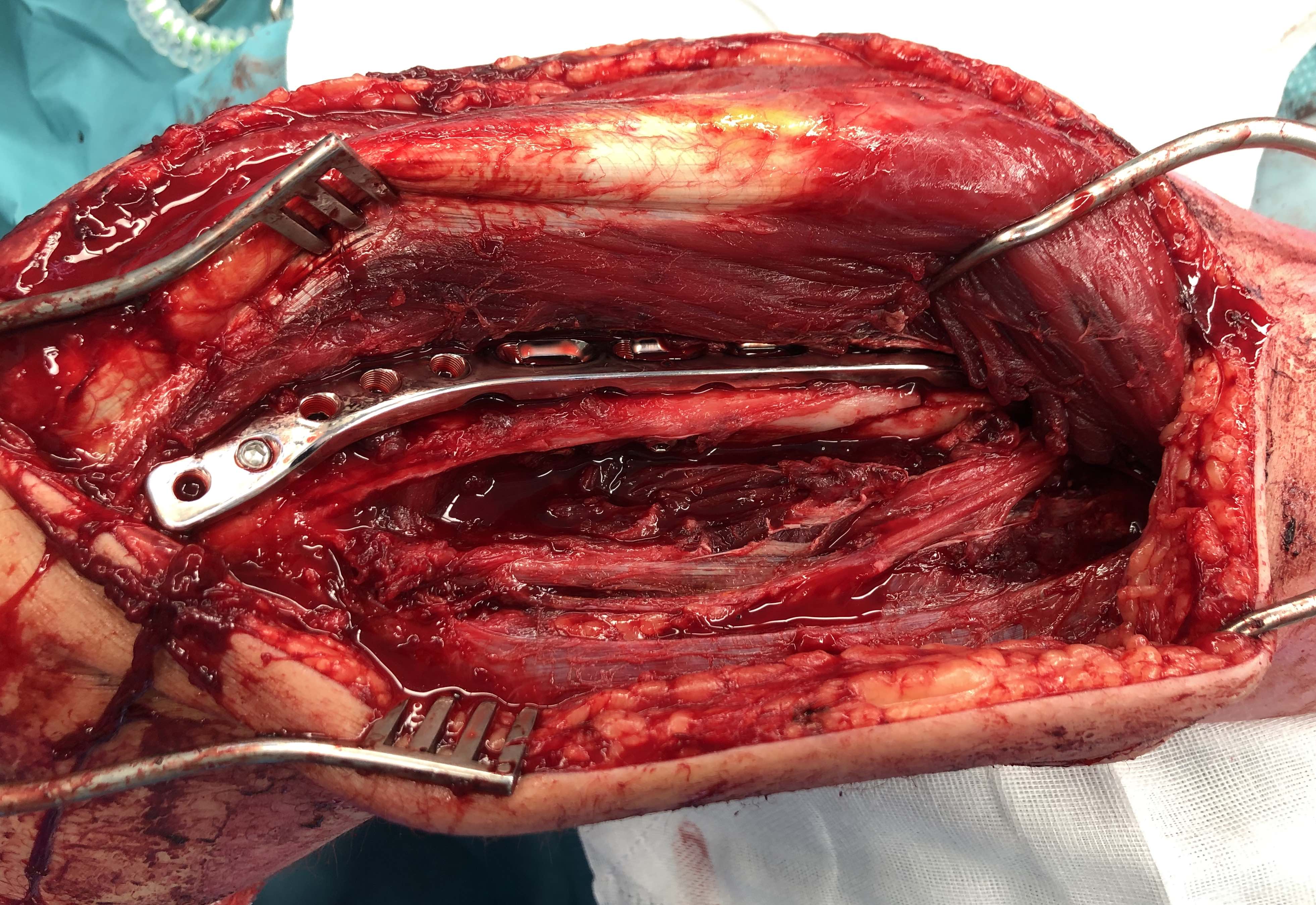
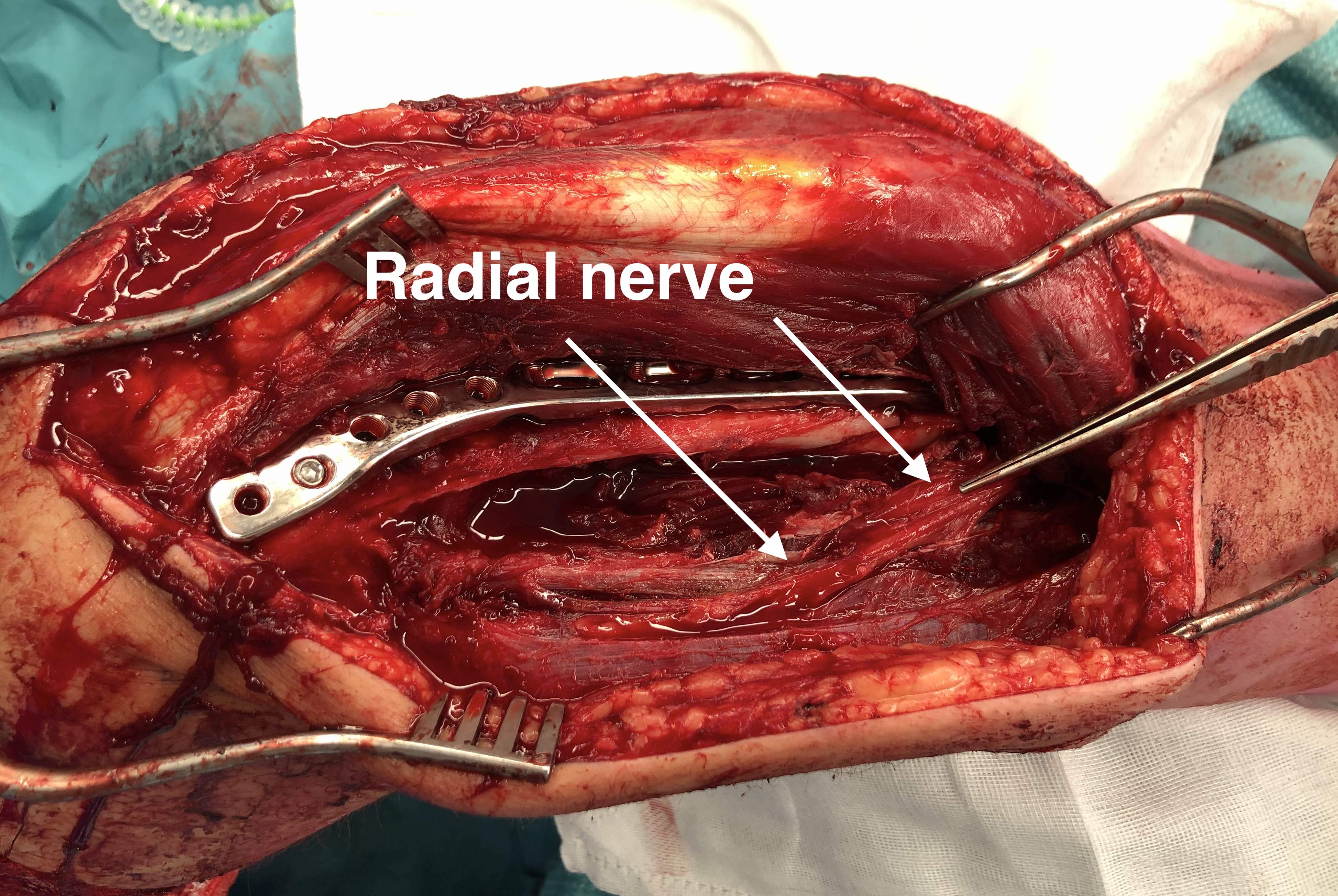
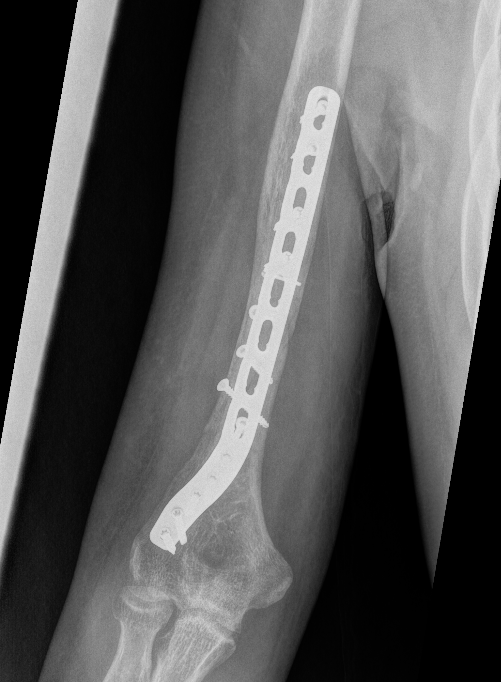
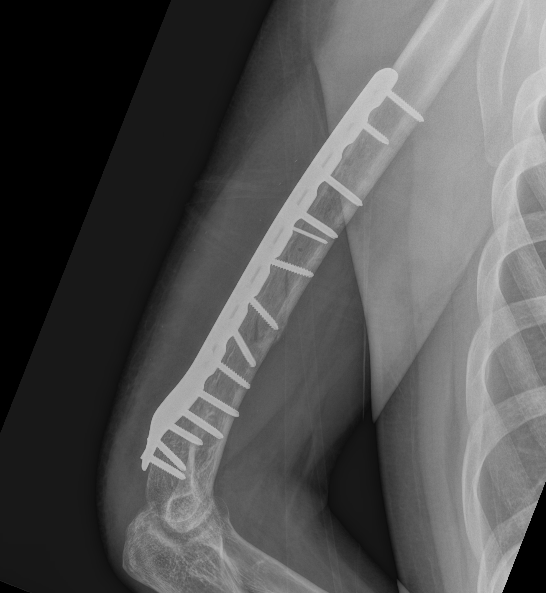
Posterolateral plate
B. Proximal window between long and lateral heads
- slide plate under radial nerve
- fix with screws proximal and distal
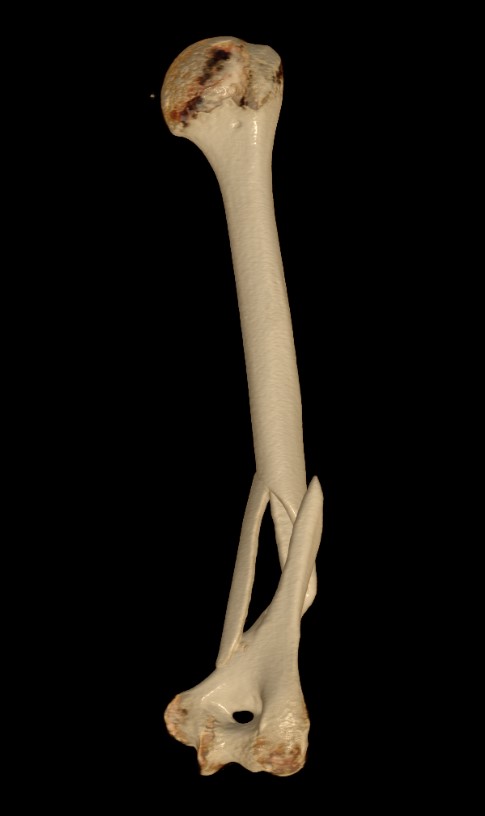
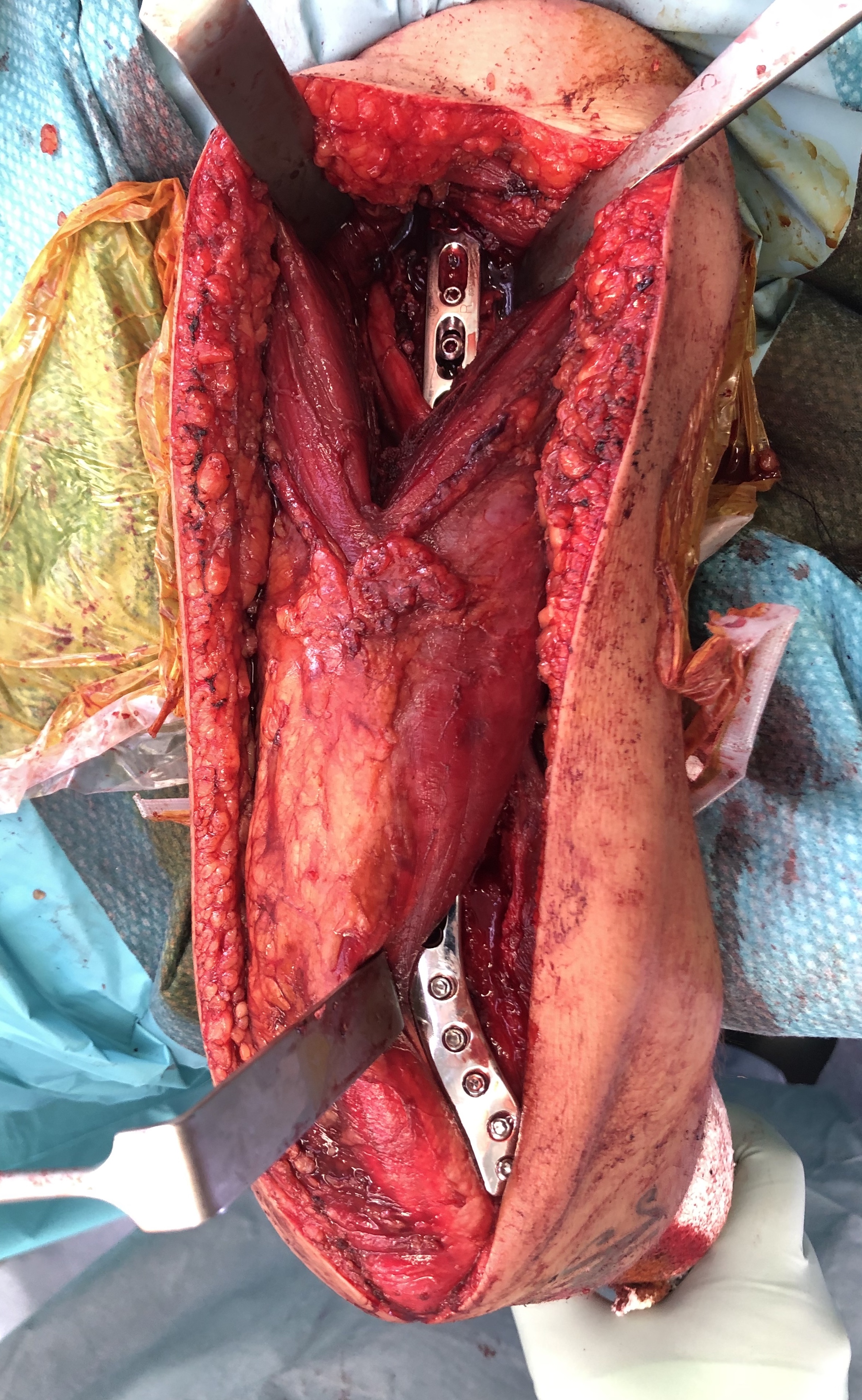
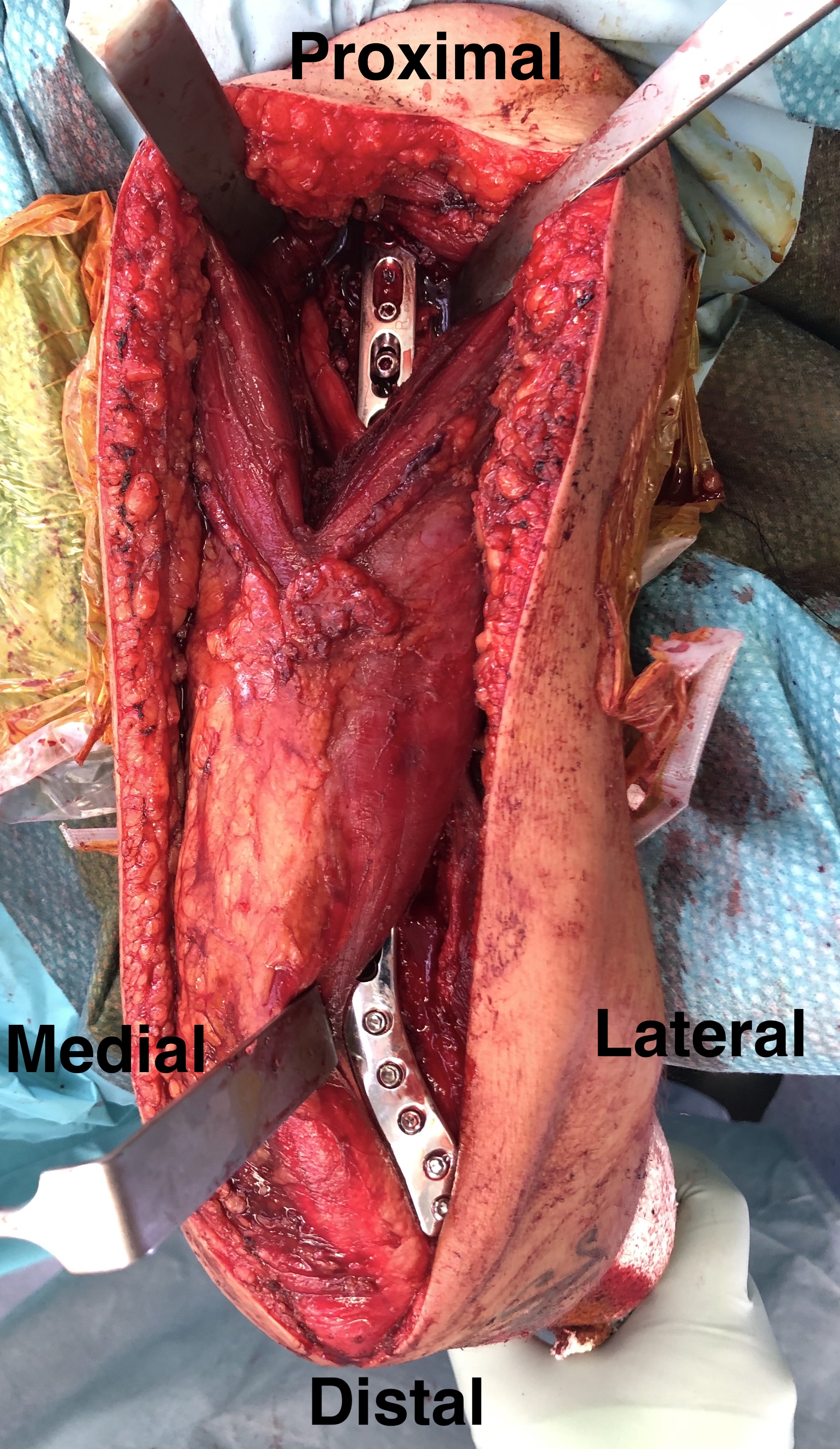
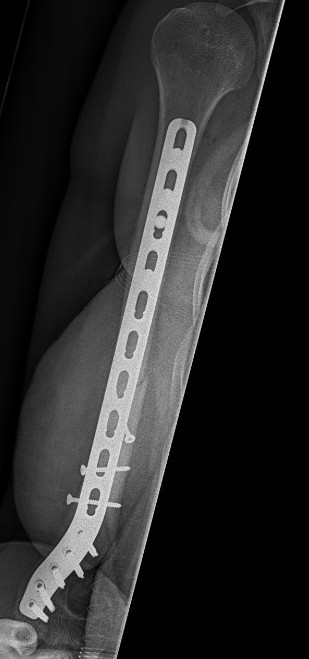
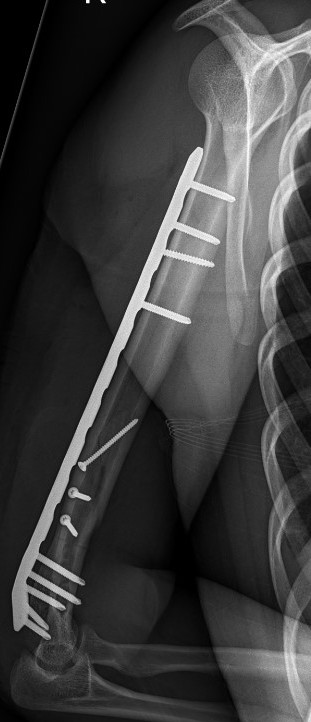
C. Can also mobilise medial triceps
- identify and release the ulna nerve medially
- additional medial plate if needed
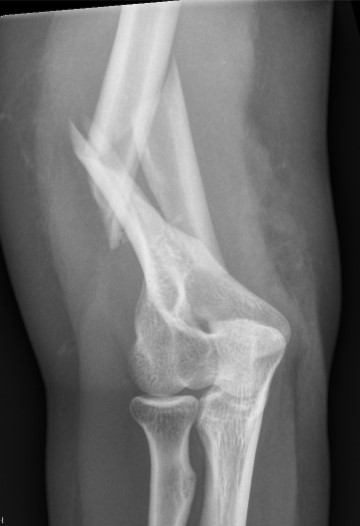
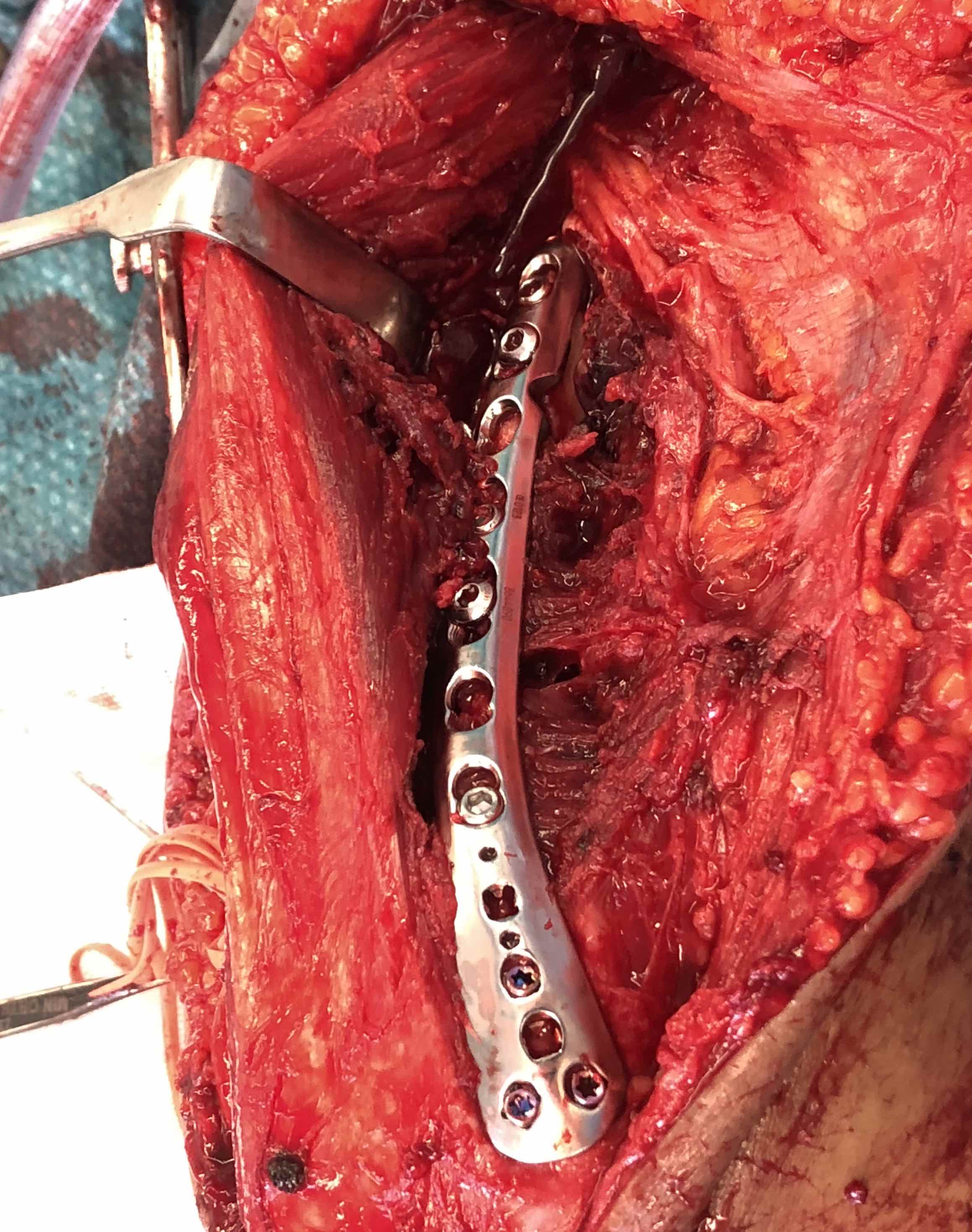
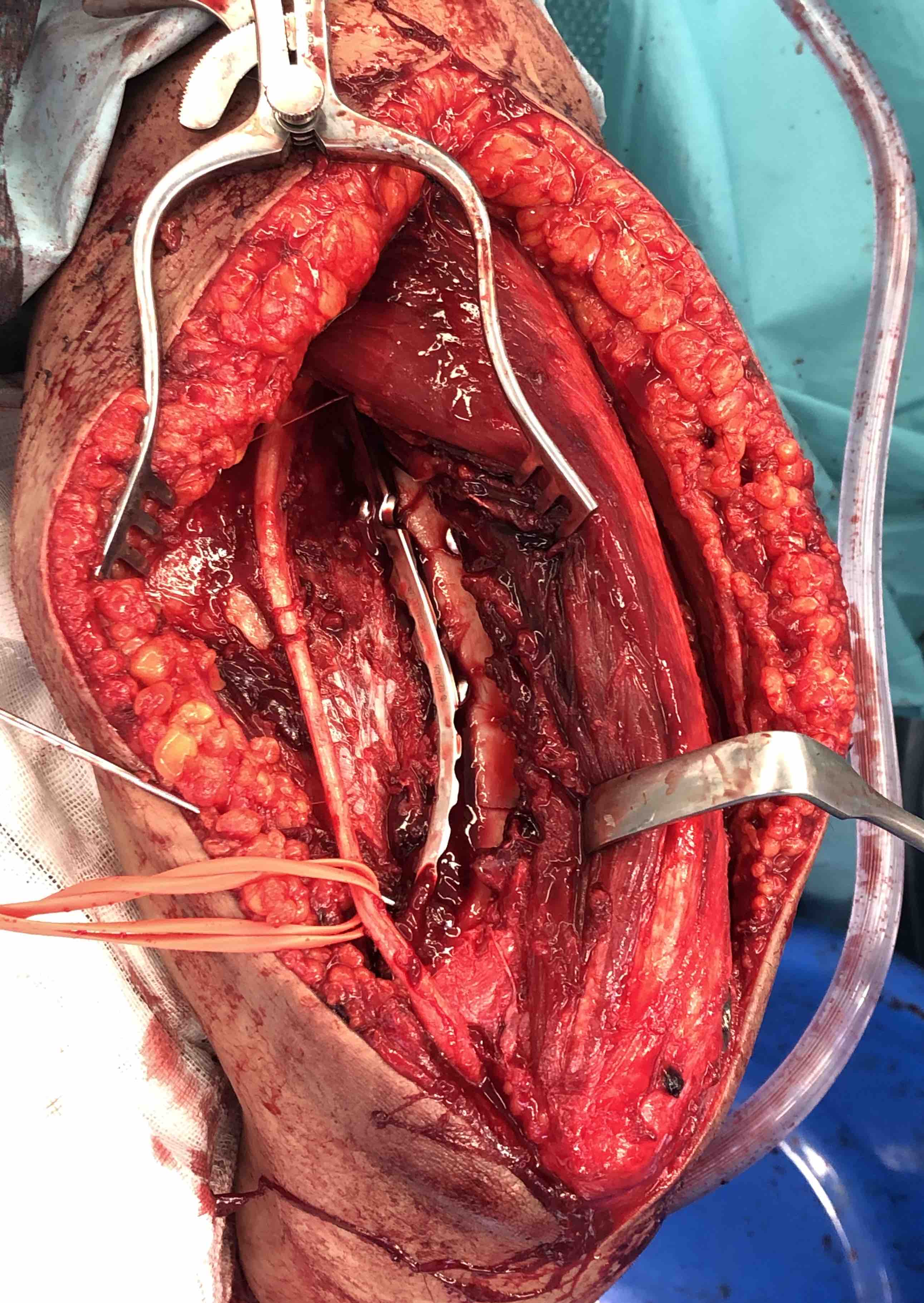
Distal humerus fracture Lateral plate Medial plate with ulna nerve tagged
2. Minimally Invasive Plate Osteosynthesis (MIPO)
Concept
Bridge plating
Indirect fracture reduction
Indications
Surgical neck of humerus to 10 cm of elbow joint
Options
Anterior plating with narrow 4.5 mm LCP
Lateral plating with long proximal humerus plate
Jeong et al. BMC Musculoskeletal Disorders
- 18 patients treated with narrow LCP (anterior)
- 17 patients treated with long Philos plate (lateral)
- 2 metal failures in the Philos plate group requiring revision to LCP
Technique anterior MIPO plating
Position
- patient supine
- arm on arm table
- ensure can image proximal humerus
- keep elbow flexed to aid reduction and reduce biceps tension
Narrow LCP plate
- place on arm to select appropriate size
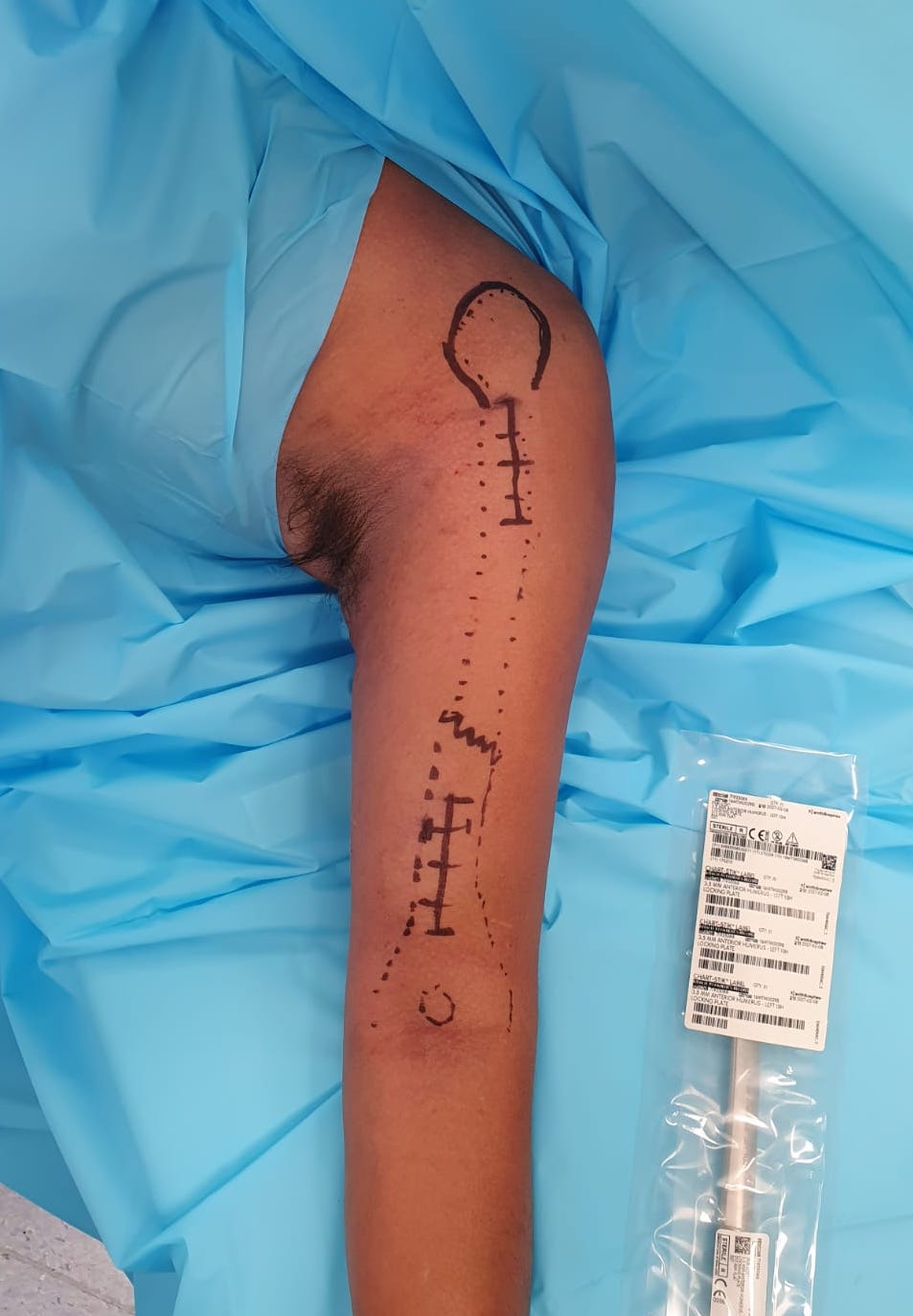
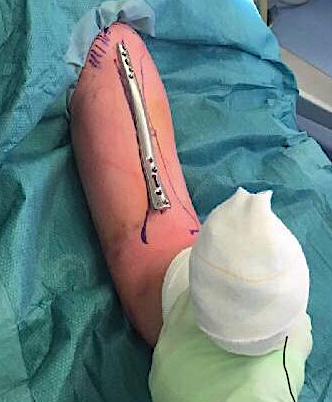
Incisions
Proximal 4 - 5 cm
- deltopectoral approach
Distal 4 - 5 cm
- anterior approach to distal humerus
- mobilise biceps laterally
- identify and protect lateral cutaneous nerve of the forearm
- split bracialis
- keep arm supinated to protect radial nerve
- avoid deep retractors laterally to protect radial nerve
Create submuscular plane
- periosteal elevator along bone
Precontour narrow LCP plate
- subtle convex curve proximally
- subtle concave curve distally
- 10 - 15 degrees internally rotated
Pass plate
- indirect fracture reduction
- secure plate proximally to bone
- reduce fracture
- distal fixation
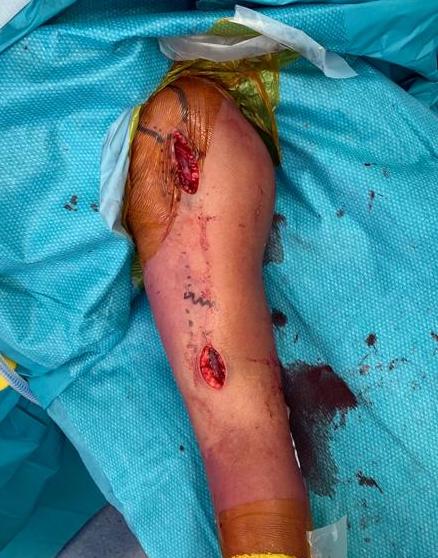
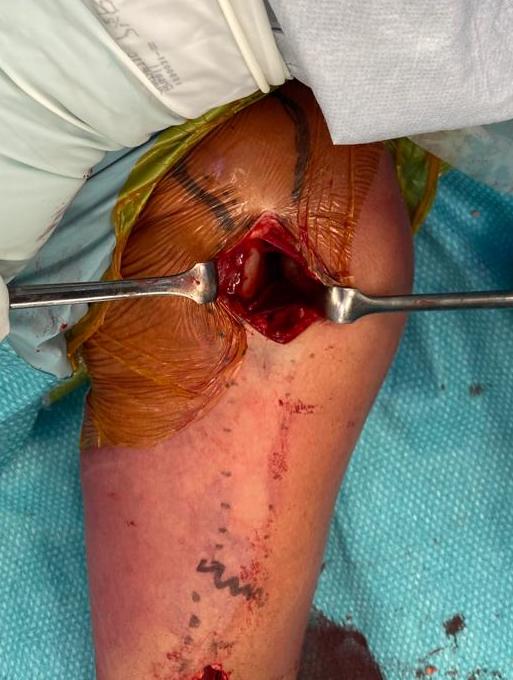
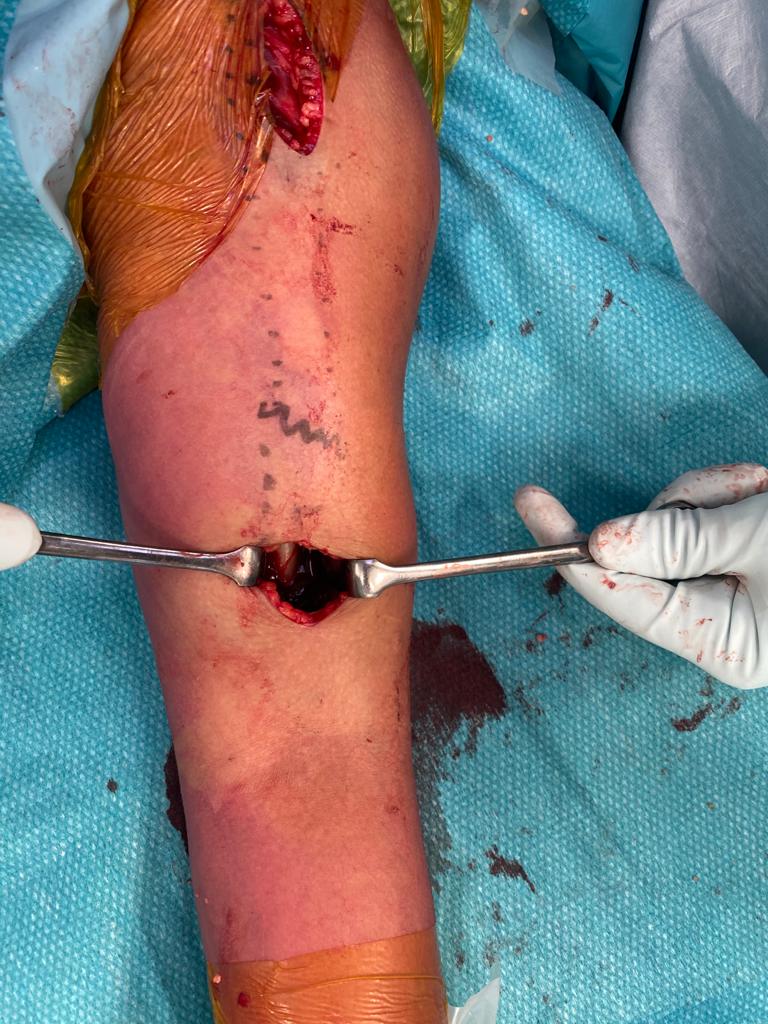
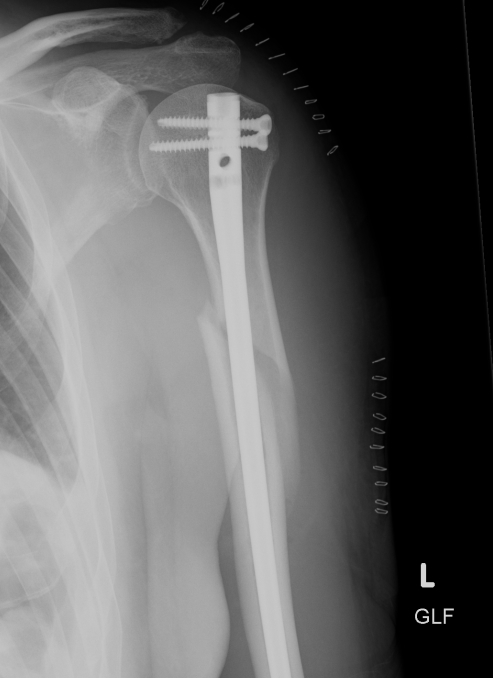
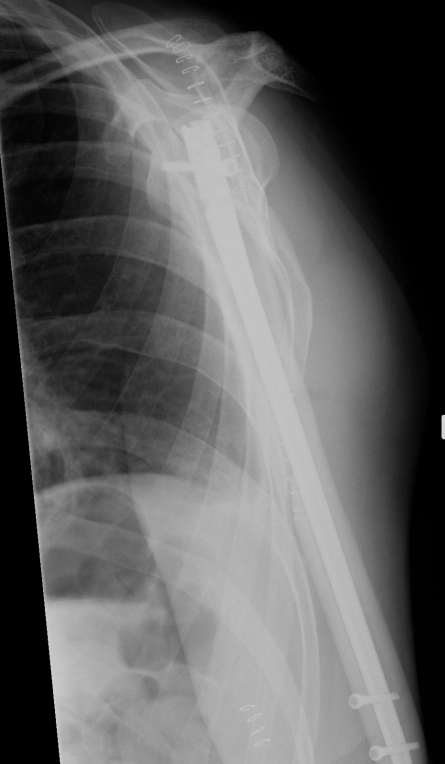
3. Antegrade Humeral Nail
Relative indications
Segmental fracture - need very long plate
Impending pathological fracture
Obesity
Skin compromise
Technique
Set up
- lazy beach chair
- can do flat on bed, with bump under shoulder
- need to get fluoroscopy of shoulder and distal forearm
- have fluroscopy come from opposite side
- patient relatively supine to ensure ease of AP distal locking
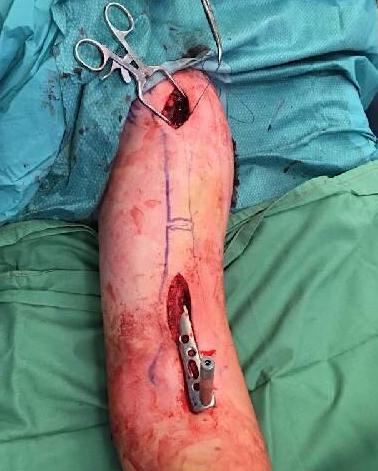
Anterolateral approach shoulder
- longitudinal split supraspinatus
- can split at the anterior edge of supraspinatus, and retract posteriorly
- protect rotator cuff throughout
Entry with K wire or awl
- entry point at medial aspect greater tuberosity
- theorectically protects the cuff tendon
- check centred in humerus canal using fluoroscopy on AP and lateral
- increase diameter proximally with hand reamers
Pass guide wire
- can do closed
- can perform mini open incision over fracture site
- use finger to blunt dissect and protect radial nerve
Minimal reaming
Pass nail
- typically 7 mm
- ensure that nail is buried enough to protect cuff
- need to consider hardware removal
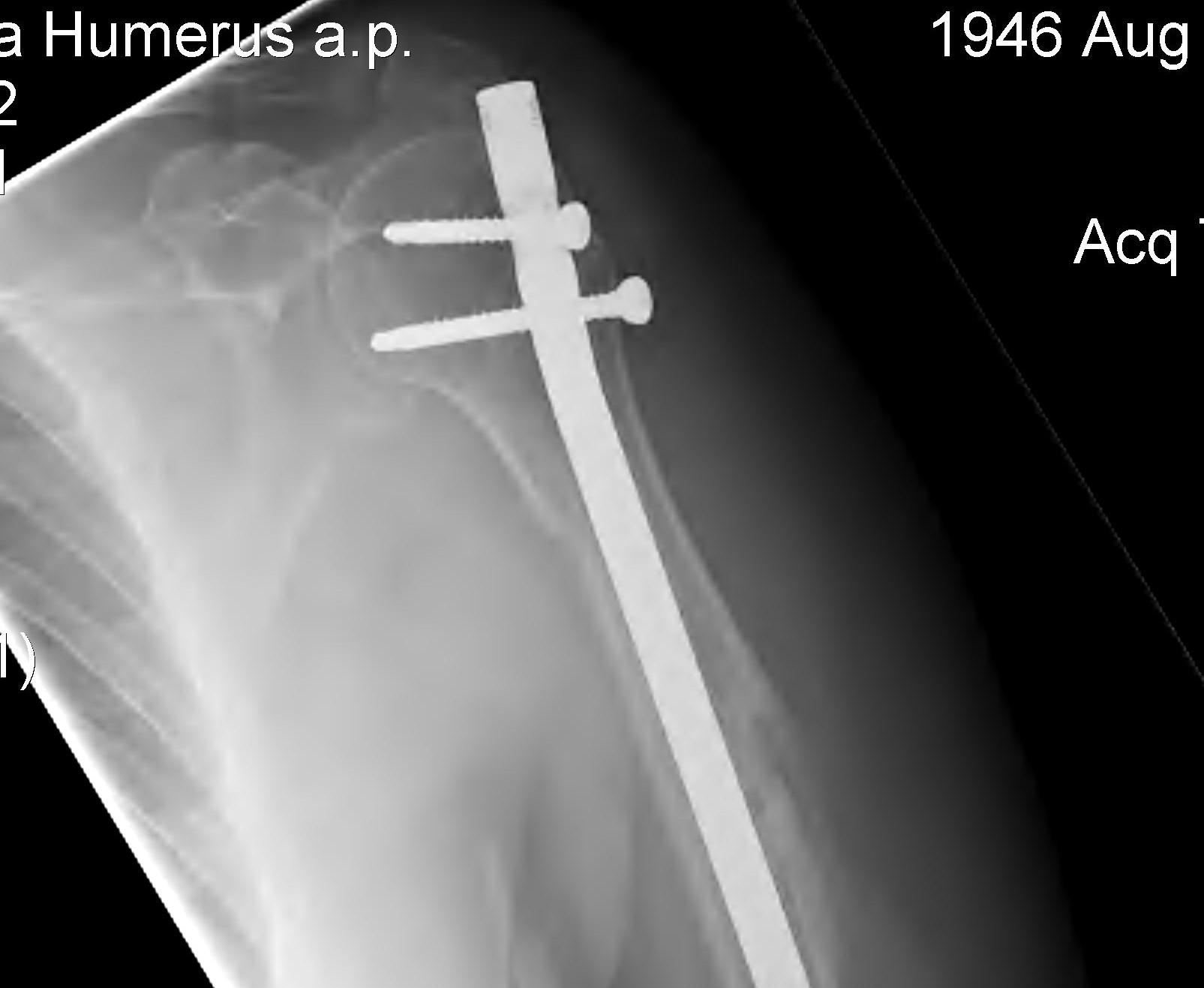
Proximal locking screws
- ensure not in joint
- lateral and anterolateral
- protect biceps tendon
Distal AP locking screw/s
Careful repair of rotator cuff
Complications
Rotator cuff pain
- must not leave nail prominent
- must carefully repair cuff
Non Union
Background
Definition
Mean time to union is 13 weeks
No evidence of callous on xrays taken 6 - 8 weeks apart
Fracture patterns
- highest risk is transverse fractures
- proximal humerus shaft fractures also at risk due to displacing force of pectoralis and deltoid, and LHB may interpose
Management
- systematic review of union rate after operative intervention of humeral shaft non union
- plate only 95%
- plate and bone graft 98%
- IMN 66%
- IMN + bone graft 88%
- external fixation 98%
Technique
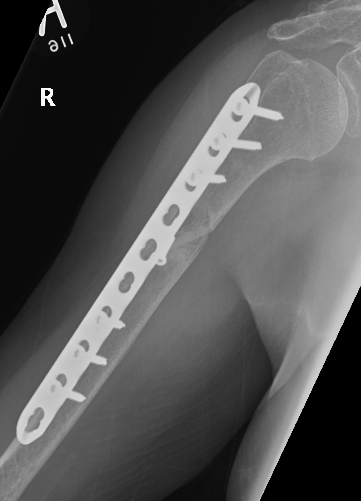
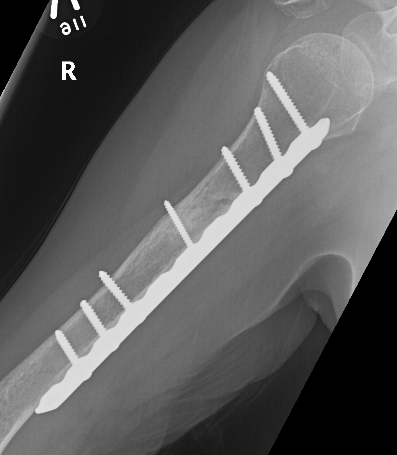
Approach
- fracture site dependant
- 4.5 mm plate with 6 cortices above and below
- if use 3.5 mm long proximal humeral plate, suggest 8 cortices below
- use iliac crest bone graft
- consider dual plating in proximal fractures with insufficient fixation, or in poor bone quality
Infection