infection
Complications
Complications
Subscapularis failure
Rotator cuff failure
Instability
Infection
Periprosthetic fracture
Aseptic loosening
Neurological injury
Parada et al. J Should Elbow Surg 2021
- 2224 aTSA complication rate 11%, revision rate 5.6%
Complications
General
- haemarthrosis
- DVT
- infection
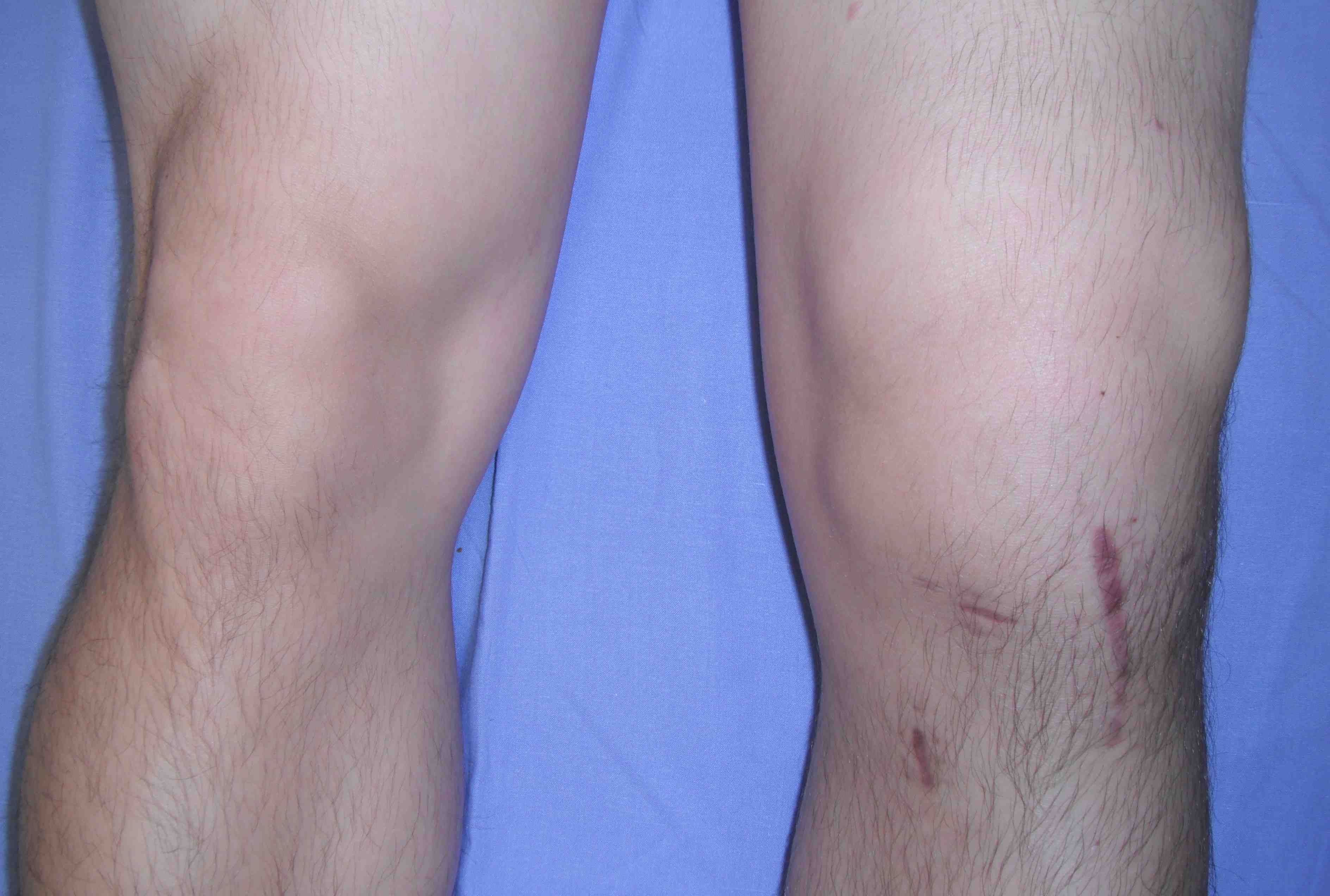
Septic Arthritis
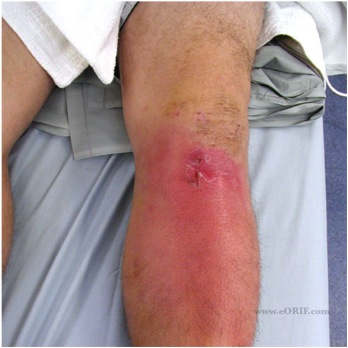
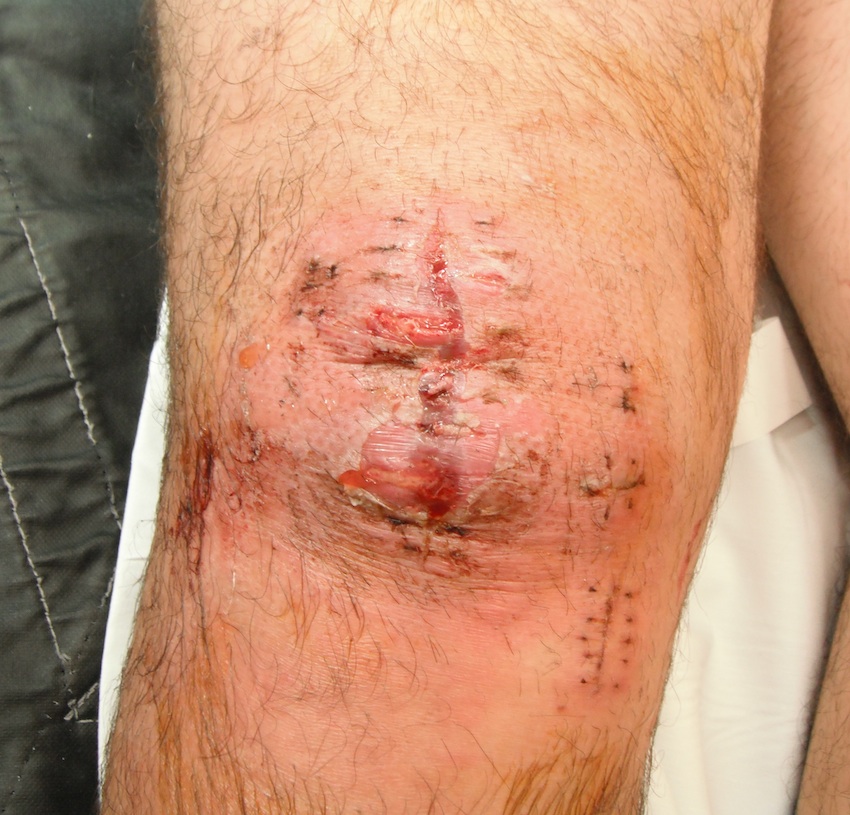
Incidence
Complications
1. Infection
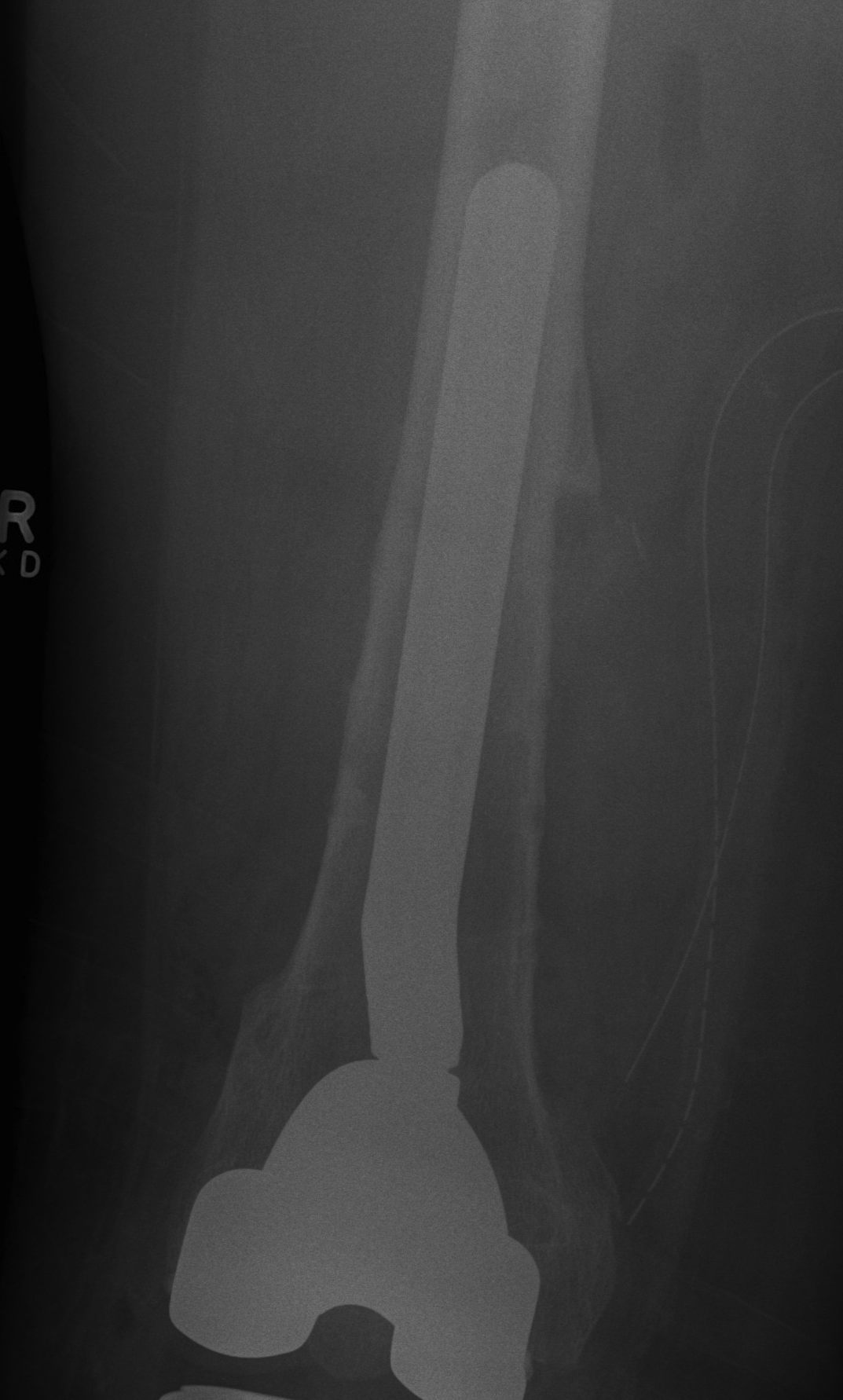
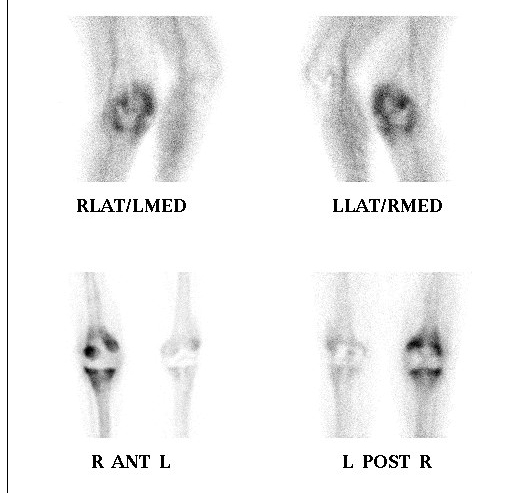
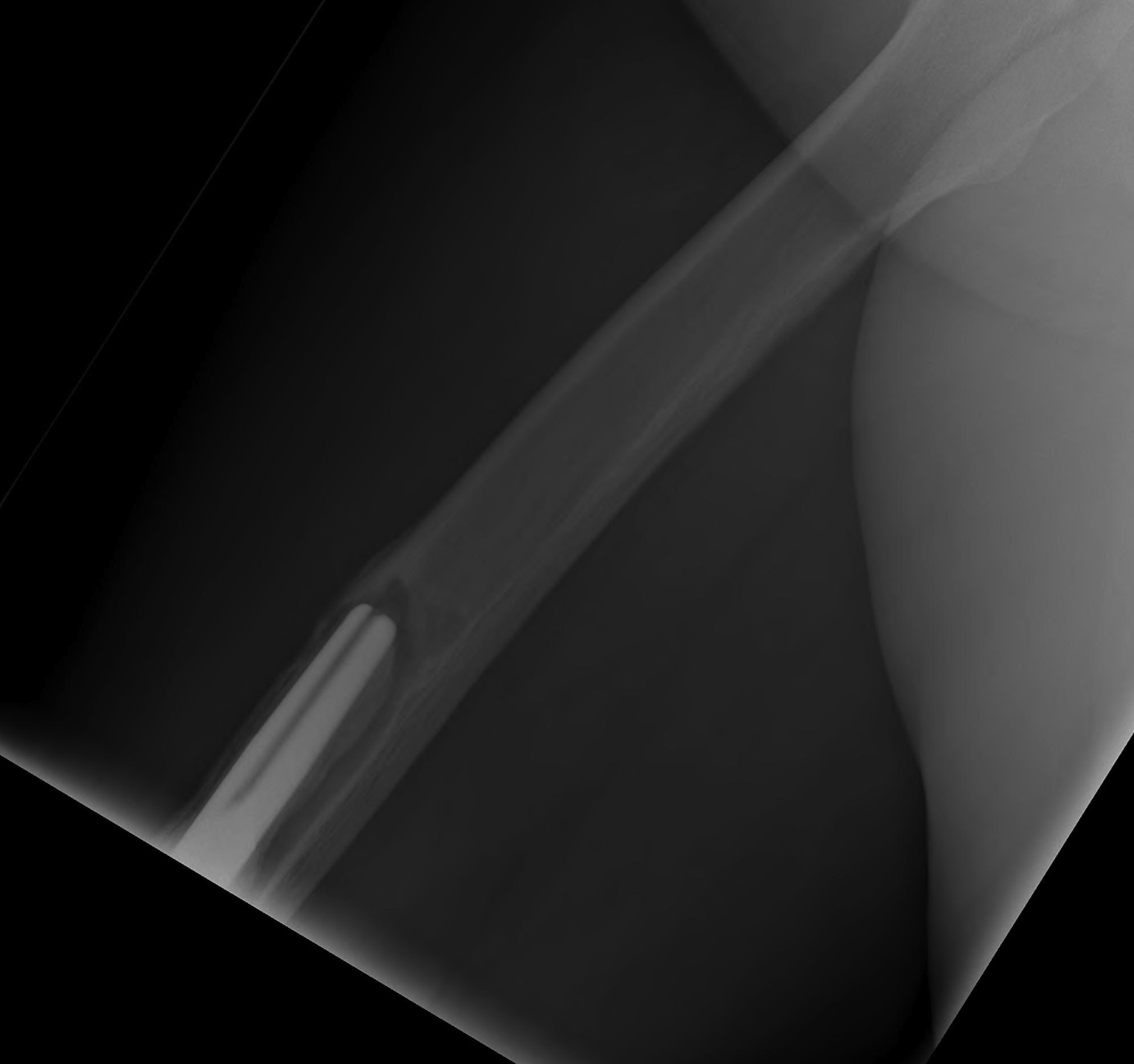
Peters et al J Arthroplasty 2009
Management
Incidence
Knee > Hip
- superficial position
- limited cover of well vascularised muscle
- watershed area of skin blood supply anterior to the skin incision
- much increased in fully constrained prosthesis
Ideal < 1%
Risk Factors
Increased with
- revision
- prior infection
- RA / Psoriatic arthropathy
- DM
Prevention
Preoperative
Identify high risk groups
- immunocompromised
- diabetes
- RA
- malnutrition
Urine screen
- check for and treat UTi
Groin, nose, axilla swabs
- for MRSA
- if positive, treat
- need 3 consecutive free swabs
3 x chlorhexidine preoperative showers in 8 hours
Admit day of surgery
- check skin for lesions
Complications
Undercorrection / loss of correction
Most important factor in good results and duration of results
- must correct to 8o of valgus
- mechanical axis must pass through lateral joint line
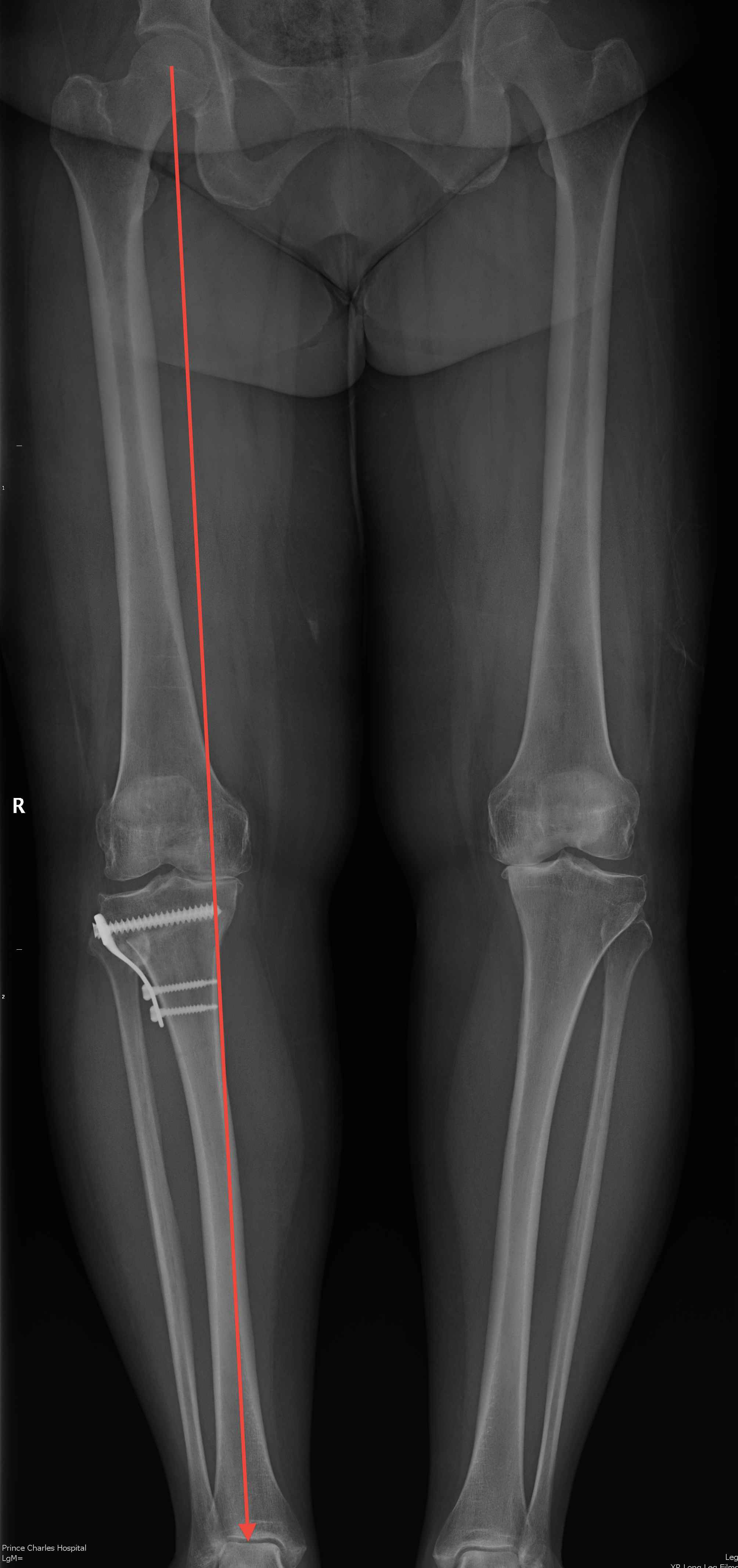
Causes
- inadequate initial correction
Intertrochanteric Fractures
Definition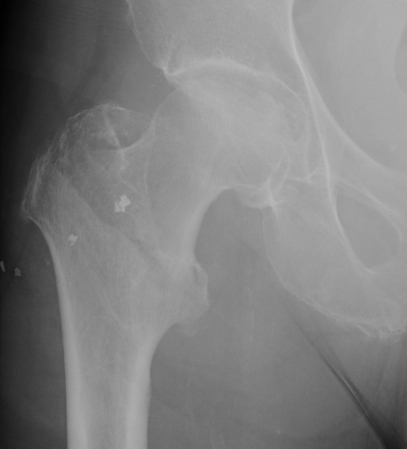
Fracture which extends between the trochanters of the proximal femur
- lower limit is inferior border of lesser tuberosity
Anatomy
Extra capsular / well vascularized
The key to stability is the posteromedial cortex
Complications
Intraoperative glenoid fracture
Avoid by
- careful reaming and drilling osteoporotic bone
Management
1. Rotate metaglene
- use locking screws to stabilise glenoid
2. PA screws
- cannulated 4.0 mm screws
- inserted percutaneously from posterior
Haematomas
Great deal of dead space is created
- always use a drain
